Dermaplaning: The Secret to Smooth, Radiant Skin
This article is written by experienced Physician Assistants Bridget Lolli, PA-C and Nancy Conley, PA-C of Aesthetic Dermatology, who are passionate about helping patients achieve their healthiest, most radiant skin through safe, customized care.

Bridget Lolli

Nancy Conley
If you’ve ever wondered how celebrities manage to have that flawless, glowing, camera-ready skin—let us let you in on a little secret: dermaplaning. This simple yet powerful treatment has become one of our go-to options for patients who want instantly smoother skin without any downtime.

So, What Exactly Is Dermaplaning?
In the simplest terms, it’s a physical exfoliation treatment that uses a sterile surgical blade to gently remove dead skin cells and that fine vellus hair we often call “peach fuzz.” It’s completely painless, surprisingly relaxing, and incredibly effective.
Throughout the day, dead skin cells build up on your skin’s surface, dulling your natural glow and making it harder for your skincare products to absorb. Peach fuzz can also affect how smoothly makeup applies and wears. Dermaplaning gives your face a clean slate: products sink in better, foundation glides on more evenly, and your complexion looks instantly refreshed.
Our Signature Touch
At our clinic, we take it a step further. Each dermaplaning session includes an enzyme exfoliation to sweep away any lingering debris and a custom mask tailored to your skin’s needs—whether that’s hydration, calming, or brightening. You leave with skin that feels baby-soft and looks lit-from-within.
And no—this treatment will not make your hair grow back darker or thicker. That’s a common myth. The hair grows back just the same—only softer at the tip.
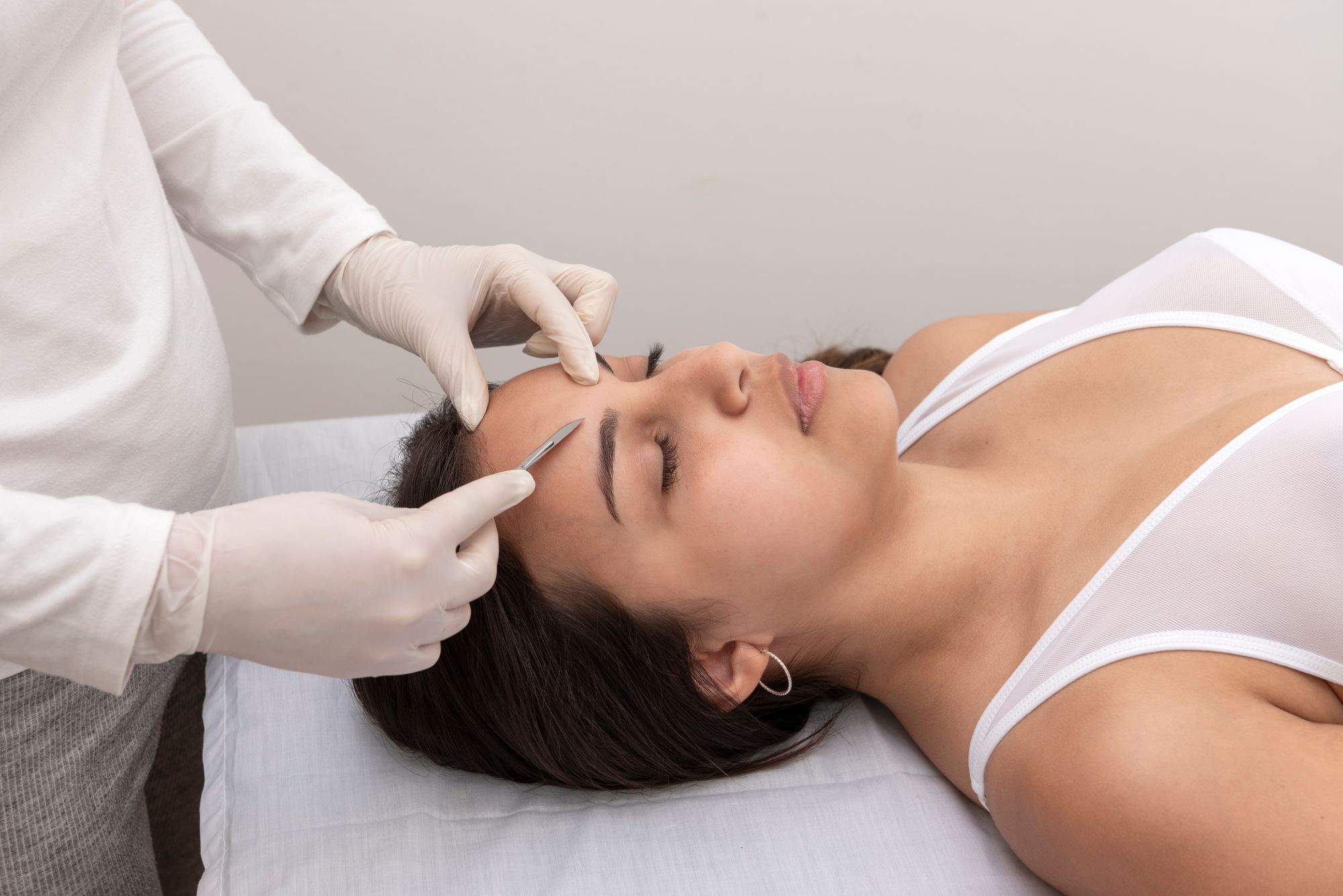
Interesting Facts About Dermaplaning
-
It’s not just for women – Plenty of men love dermaplaning too (yes, even those with beards benefit from cheek and forehead treatments).
-
It boosts product performance – Without that layer of dead skin, serums and moisturizers absorb more effectively.
-
Makeup artists swear by it – Many do it before photoshoots or red carpet events to get that perfect canvas.
-
It’s safe during pregnancy – Dermaplaning is a gentle, non-invasive option that’s often recommended during pregnancy.
-
You can combine it with other treatments – It pairs beautifully with facials, LED therapy, and more.
What You Should Know Before Getting Dermaplaning
-
It’s quick and relaxing – A session typically lasts around 30–45 minutes, and there’s no downtime.
-
It’s great for most skin types – Including sensitive skin, rosacea, or those with pigmentation concerns.
-
It’s not painful at all – Most people say it feels like a gentle brushing sensation.
-
It’s best done every 3–4 weeks – That’s about how long your skin needs to regenerate.
What to Avoid Before Dermaplaning
To get the best results from your treatment, here are a few things to avoid:
-
Avoid retinoids or exfoliants for 2–3 days beforehand.
-
Skip any waxing or threading in the dermaplaning area one week before.
-
Avoid sunburns or active breakouts, as irritated skin isn’t a good match for dermaplaning.
-
Hold off on recent chemical peels – Your skin should be calm and not recently exfoliated.
Who Shouldn’t Do Dermaplaning
While dermaplaning is safe for most, it’s not for everyone:
-
Active acne – The blade can aggravate inflammation and spread bacteria.
-
Cystic acne or open wounds – It’s best to wait until your skin is healed.
-
Severe rosacea or eczema – Dermaplaning may trigger a flare-up.
-
Overly sensitive skin post-treatment – If you’ve recently had a strong peel or laser treatment, give your skin time to recover.
Feeling nervous or unsure about trying a cosmetic treatment for the first time? That’s completely normal—and we’re here to help. If you’re wondering whether dermaplaning is right for your skin, our team is always happy to answer your questions, evaluate your skin, and recommend the best treatment plan for your goals.

Bottom Line: Glowing Skin Is One Blade Away
Dermaplaning is ideal before big events, photo shoots, or simply when you want your skin to look its absolute best. It’s safe, effective, and a client favorite for a reason.
Never tried it? Now’s the perfect time.
👉 Book your dermaplaning appointment at one of our convenient locations in Paoli or Media—and let’s get your glow on.
Expert Acne Treatments You Can Only Get From a Dermatologist
Why Acne Happens — and to Whom
Acne is a complex skin condition that can affect people of all ages—not just teenagers. While it’s most common during puberty, due to hormonal fluctuations, adult acne is on the rise and often tied to factors like stress, hormonal imbalances, or skincare habits.
Several underlying causes can contribute to breakouts: hormonal changes, especially during adolescence, pregnancy, or menstrual cycles; genetics (if your parents had acne, you’re more likely to experience it too); diet, particularly high-glycemic foods like sugary snacks, white bread, and dairy; and lifestyle factors such as stress, poor sleep, or heavy use of oily cosmetics. Environmental influences like humidity, sweat, and pollution can also aggravate acne-prone skin.
No two cases are exactly alike, which is why personalized care from a certified dermatologist can make such a difference.

Prescription-Strength Topical Treatments
These formulations contain higher concentrations of active ingredients compared to drugstore options and are tailored to your skin’s unique needs.
- Retinoids (like tretinoin, adapalene, and tazarotene) help unclog pores, reduce inflammation, and promote skin cell turnover.
- Topical antibiotics, such as clindamycin and erythromycin, combat acne-causing bacteria and calm redness.
- Azelaic acid offers anti-inflammatory and antimicrobial benefits while also helping to lighten dark spots left by acne.
Prescription Oral Medications
For more severe acne, especially when inflammation or hormonal imbalances are involved, oral treatments can be highly effective.
- Oral antibiotics (e.g., doxycycline or minocycline) reduce inflammation and bacteria from within.
- Hormonal therapy like spironolactone can be especially helpful for women with hormonally driven breakouts.
- Isotretinoin (commonly known as Accutane) is a powerful, transformative treatment for severe cystic acne—but it requires careful monitoring by a dermatologist due to potential side effects. I often guide patients through this journey safely and with long-term results in mind.
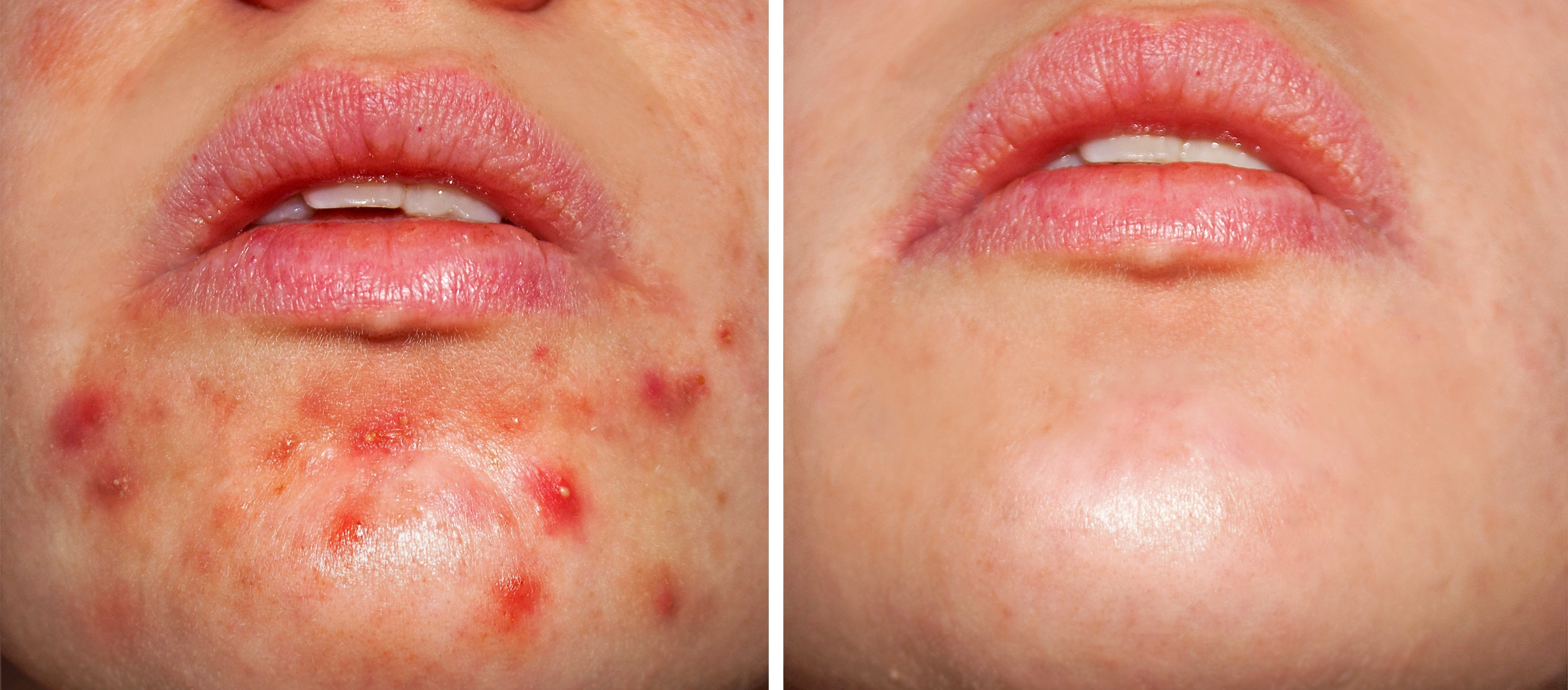
Acne treatment – before and after.
In-Office Procedures for Quicker Results
Dermatologists offer a range of advanced procedures that accelerate acne clearance and improve skin texture:
- Chemical Peels: Medical-grade peels using salicylic acid, glycolic acid, or trichloroacetic acid (TCA) help exfoliate the skin, unclog pores, and fade acne scars.
- Laser and Light Therapy: Blue light and intense pulsed light (IPL) therapy kill bacteria and reduce inflammation, while laser treatments target deeper layers of the skin to improve acne scars.
- Steroid Injections: For painful, deep cystic acne, dermatologists can inject corticosteroids directly into lesions to rapidly shrink them within 24-48 hours.
- HydraFacial and Microdermabrasion: These treatments deeply cleanse pores and remove dead skin cells, reducing breakouts and blackheads.
Personalized Acne Scar Treatments
Even after acne clears, scars and hyperpigmentation can linger. Dermatologists offer cutting-edge solutions like:
- Microneedling with PRP (Platelet-Rich Plasma): Uses tiny needles to stimulate collagen and heal scars.
- CO2 and Fractional Laser Resurfacing: Smooths out deep acne scars by promoting new skin cell growth.
- Dermal Fillers: Used to lift depressed acne scars for a more even skin texture.

What Not to Do After Acne Treatment
Treating acne is just the first step—maintaining results requires ongoing care and avoiding certain common mistakes.
- Don’t stop treatment prematurely. Many patients feel better after a few weeks and stop their regimen too soon. Acne is a chronic condition for many people and requires consistency.
- Avoid picking or squeezing blemishes, which can lead to more inflammation, scarring, and pigment changes.
- Don’t overload your skin with too many products—especially harsh scrubs, alcohol-based toners, or “miracle cures” trending online. These can irritate the skin and worsen acne.
- Avoid tanning beds or unprotected sun exposure after procedures like peels or lasers. Sun damage can hinder healing and cause pigment changes.
- Stick to a dermatologist-approved skincare routine, including gentle cleansers, non-comedogenic moisturizers, and sunscreen.
A healthy lifestyle—balanced diet, regular sleep, and stress management—also goes a long way in keeping acne at bay.
Why See a Dermatologist for Acne Treatment?
Dermatology is more than just treating symptoms—it’s about understanding the why behind your acne and creating a plan tailored to your skin and lifestyle. Whether you’re dealing with hormonal acne, persistent cysts, or long-standing scars, I work closely with each patient to find what truly works for them.
If you’ve been cycling through countless products without success, I encourage you to schedule a consultation. There’s no one-size-fits-all answer, but with expert guidance, long-term results are absolutely possible.

Ready to Take the Next Step Toward Clearer Skin?
If you’re dealing with acne or other skin concerns, expert help is just a click away. I offer comprehensive dermatologic care through convenient telehealth appointments, allowing you to receive a personalized consultation, treatment plan, and follow-up—all from the comfort of your home.
Whether you’re managing persistent breakouts, exploring prescription options, or looking for guidance on skincare routines, my virtual practice makes high-quality dermatology accessible and efficient.
Don’t wait to get the care you need—schedule your online consultation today and take the first step toward clearer, healthier skin with a board-certified dermatologist you can trust.
Eczema Relief: Best Medical and At-Home Treatments for Fast Recovery

By Dr. James Ko, MD, Board-Certified Dermatologist
If you are living with eczema, you already know how difficult and frustrating it can be. The itching, dryness, redness — sometimes it feels like it never ends.
As an experienced eczema dermatologist, I am Dr. James Ko, and I want to share with you the real ways we can achieve faster and deeper relief, based on the latest medical research and clinical practice.
Understanding Eczema and Why Personalized Treatment Matters
Eczema, or atopic dermatitis, is not just dry skin or a simple rash.
It is a complex inflammatory disorder, involving a combination of immune system dysfunction, defective skin barrier, and environmental triggers. Genetic factors also play a strong role.
Many patients think moisturizing is enough. But in reality, skin hydration must go together with controlling the internal immune inflammation. Without treating both sides — outside and inside — eczema will keep returning.
This is why personalized eczema treatment is essential.
Every patient’s case is different, depending on severity, allergy history, environment, and lifestyle. No single “standard” treatment fits all.
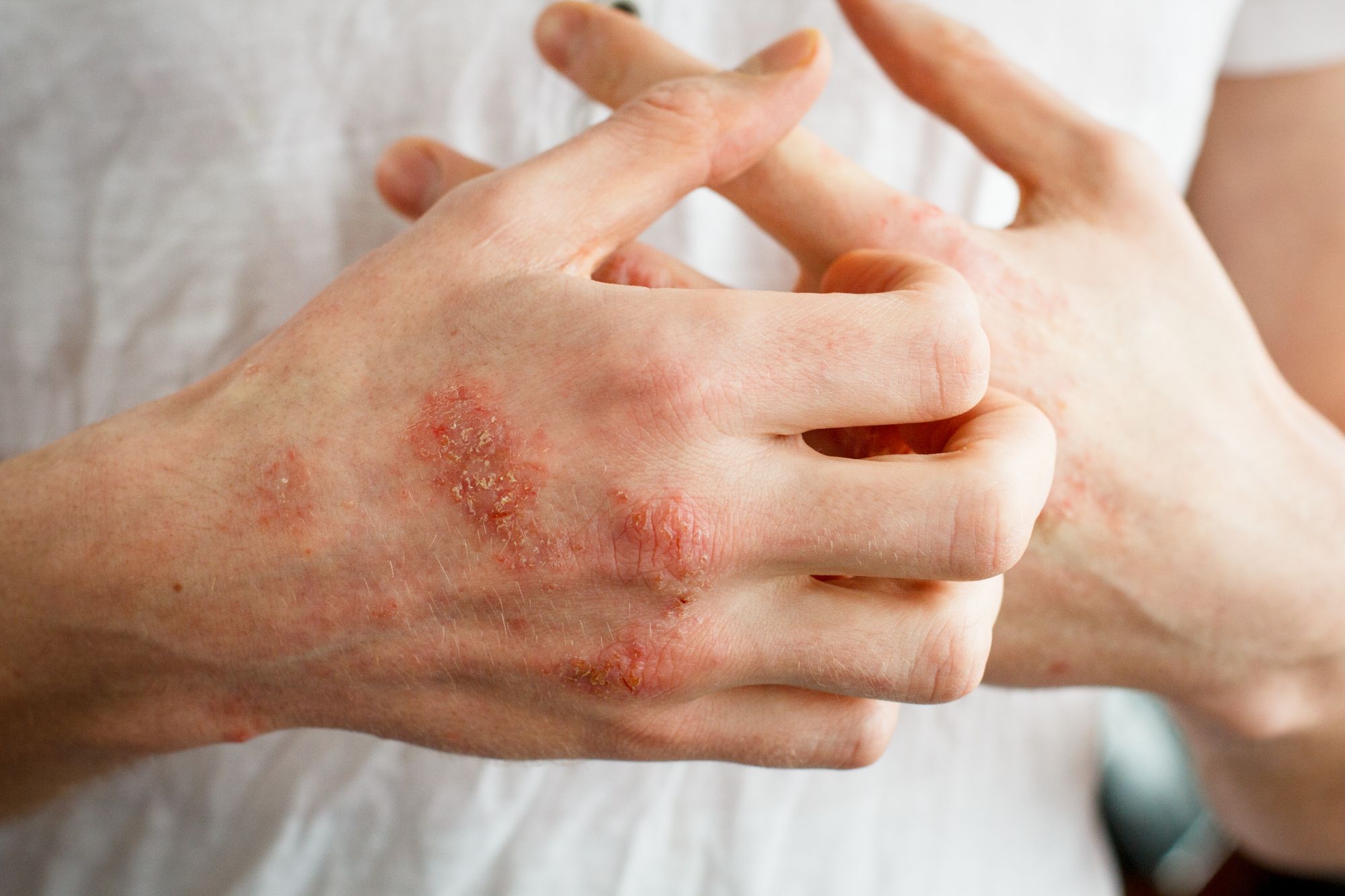
Medical Treatments Recommended by Dr. James Ko
At Aesthetic Dermatology Associates’ clinics in Paoli and Media, I recommend treatments based on the eczema’s stage (acute, subacute, or chronic) and severity (mild, moderate, or severe):
- Topical corticosteroids: Still the first-line therapy for acute flares. However, I always stress correct potency selection — for example, using low-potency steroids on the face or folds, but higher-potency steroids briefly on thick plaques. I also recommend structured “step-down” tapering after flare control, not sudden stopping.
- Prescription moisturizers and barrier creams: Eczema skin lacks certain proteins like filaggrin, causing water loss and barrier weakness. Special barrier repair creams often include ceramides, cholesterol, and free fatty acids, which mimic natural skin lipids. Using regular cosmetic moisturizers is often not enough for true barrier healing.
(Note: While I mention prescription moisturizers here, in most cases I recommend high-quality over-the-counter barrier creams or emollients that contain the right mix of ceramides, cholesterol, and fatty acids – prescription versions are only needed in more complex or resistant cases.) - Topical calcineurin inhibitors: (e.g., tacrolimus, pimecrolimus) are good alternatives when steroid side effects are a concern, especially for delicate areas like eyelids.
- Antihistamines: I prescribe sedating antihistamines mainly for nighttime use, not for daytime control. Daytime antihistamines usually do not reduce eczema itching much — this is a misunderstanding. Night use is for helping patients sleep without scratching.
- Systemic therapies (biologics and immunosuppressants): In moderate to severe cases, especially where the patient fails standard treatment, biologics like dupilumab (an IL-4/IL-13 inhibitor) are now changing how we manage eczema. I explain to patients that biologics target the immune drivers behind eczema, not only the skin symptoms.
Medical eczema treatment is not just “put some cream on and wait.” It must be dynamic, adjusted according to flare intensity and maintenance needs.
The “Soak and Smear” Method for Eczema Relief
One technique I highly recommend is the “soak and smear” approach. It can greatly accelerate recovery, especially during severe dryness or lichenified (thickened) eczema.
Here is why and how it works:
- Soaking (10–20 min in lukewarm water) rehydrates the stratum corneum (outer skin layer), making it more permeable for treatments.
- Immediate application (“smearing”) of a corticosteroid ointment or occlusive moisturizer seals water inside the skin. Research shows this increases the effectiveness of topical medications by enhancing penetration through softened skin.
- Timing is critical. Even a 1–2 minute delay between drying and moisturizing allows water loss. I advise patients to prepare everything before soaking.
The “soak and smear” method, when combined with barrier repair creams, can sometimes shorten active flare recovery by 30–40%.
At-Home Eczema Care Tips from Dr. James Ko
Many home care strategies are common knowledge, but I guide patients deeper into optimizing skin healing:
- Focus on lipid replenishment, not just hydration. Using moisturizers rich in ceramides, cholesterol, and linoleic acid rebuilds the skin structure itself, not just making it feel moist.
- Adjust your routine to weather and humidity. In dry winter months or with indoor heating, patients often need to double their moisturizing frequency. I sometimes suggest using a bedroom humidifier if ambient humidity drops below 40%.
- Short, lukewarm showers with acid-balanced cleansers. Normal soap (pH 9–10) disrupts the skin’s natural acid mantle (pH 4.7–5.5). Mild, acidic cleansers help preserve the barrier and prevent over-drying.
- Consider bleach baths (0.005% sodium hypochlorite) 2–3 times weekly for patients with secondary bacterial colonization, especially with recurrent Staphylococcus aureus infections. Clinical trials show bleach baths reduce infection and flares.
(Important: I always emphasize that bleach baths must be dilute — typically 1/4 to 1/2 cup of regular household bleach added to a full bathtub (about 40 gallons of water). Stronger concentrations can irritate or damage the skin, so proper dilution is essential for safety and effectiveness.)
Home care is not about “doing less damage” — it is about actively engineering the environment where the skin can repair itself best.
Common Mistakes That Delay Eczema Healing
Instead of simply “do not scratch,” I explain why some habits damage treatment success:
- Incomplete steroid use: Many patients underuse prescribed steroids due to fear, stopping once itching improves but before inflammation fully resolves. This leads to rebound flares. I educate patients to continue a tapering regimen even after symptoms improve.
- Ignoring secondary infections: Eczema flares complicated by bacteria or viruses (like eczema herpeticum) require different management. If a flare suddenly worsens or becomes painful, seek medical evaluation immediately — not every worsening is “just eczema.”
- Reliance on alternative therapies without supervision: Natural oils, herbal creams, and dietary changes may seem safe, but some contain allergens or irritants. “Natural” does not always mean “safe for eczema skin.”
Proper education on these mistakes saves months of unnecessary suffering.
Conditions That Are Sometimes Mistaken for Eczema
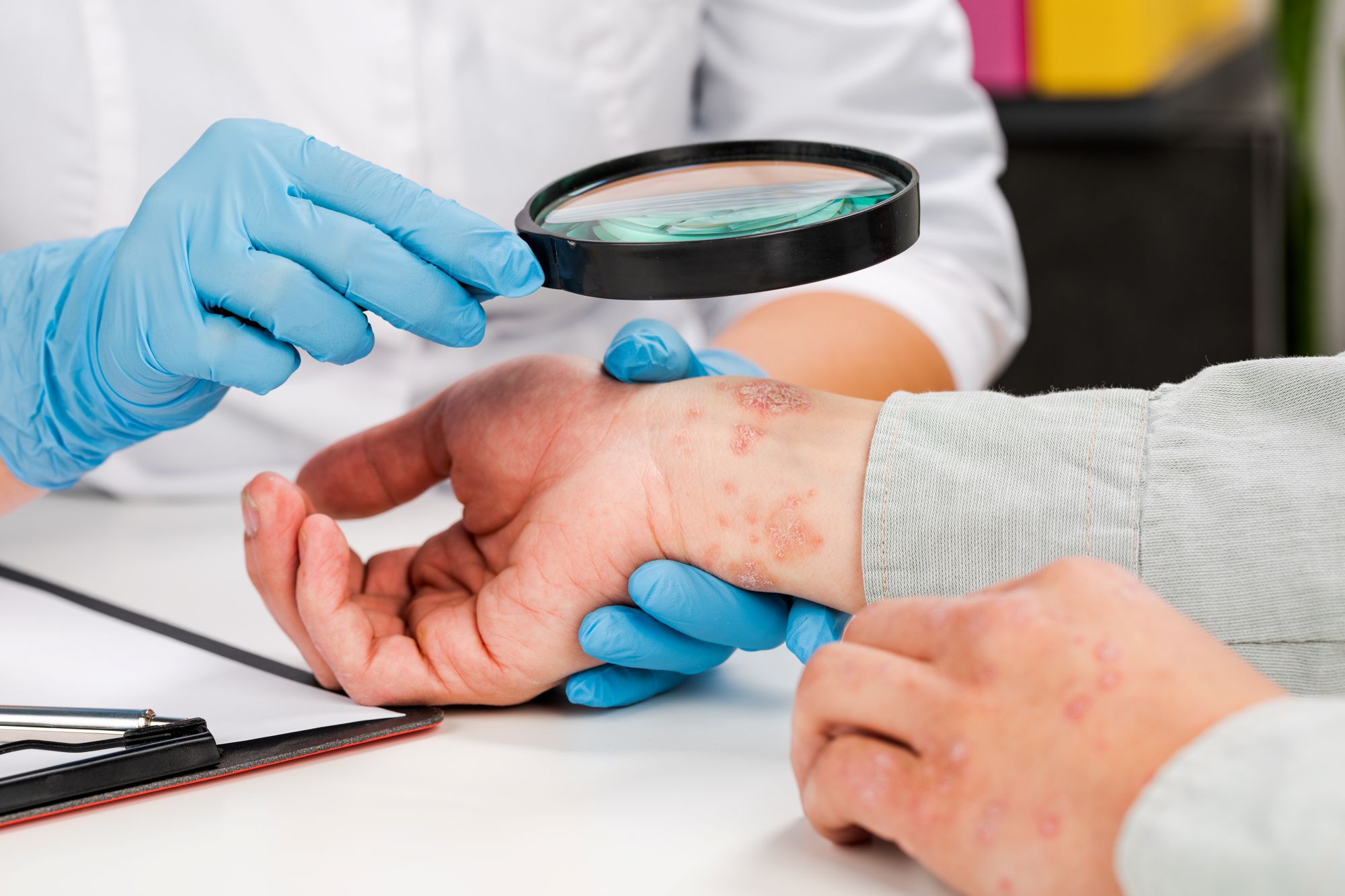
Correct diagnosis is 50% of successful treatment. Some diseases that mimic eczema include:
- Nummular dermatitis: Circular plaques resembling fungal infections. Responds to corticosteroids, not antifungals.
- Seborrheic dermatitis: Affects scalp, eyebrows, nasolabial folds — triggered by Malassezia yeast. Requires antifungal treatments alongside barrier repair.
- Tinea (fungal infections): Often misdiagnosed as eczema. I always perform KOH scraping if infection is suspected, because wrong treatment with steroids can worsen fungal disease.
- Cutaneous T-cell lymphoma (early stages): Rare but important. When eczema-like plaques do not respond to standard therapy or show atypical distribution, biopsy is necessary.
Differentiating these correctly saves time and protects patient safety.
When to See an Eczema Dermatologist
If your eczema is persistent despite using proper moisturizers and over-the-counter hydrocortisone, it is time to see an eczema specialist.
I also advise early referral when:
- Flares are interfering with work, school, or sleep.
- Signs of infection appear.
- Quality of life is affected — such as anxiety, depression from visible eczema.
- Systemic therapy might be needed.
A dermatologist can offer options beyond creams — including immunomodulators, patch testing for allergens, light therapy (narrowband UVB), and biologics.
Conclusion
Managing eczema is a partnership between the patient and doctor. It needs good planning, clear communication, and regular adjustment based on skin response.
If you are struggling with eczema despite trying your best, do not give up.
Please contact our office and schedule a consultation — together, we can create a clear, personalized eczema treatment plan and help your skin heal properly.
Mole Removal & Treatments: What You Need to Know

By Dr. Elizabeth Marvin, MD, Board-Certified Dermatologist
As a dermatologist, I frequently see patients who are concerned about changes in their moles or are simply looking for ways to improve the appearance of their skin. Whether it’s a cosmetic concern or a potential health issue, understanding when and how to address moles is important for long-term skin health.
Over the years, I’ve helped many adults and children evaluate their moles and determine the most appropriate treatment approach. In this article, I’ll walk you through what you need to know about mole removal—from what to look out for to the treatment options available.
What Are Moles?
Moles, also called nevi, are clusters of pigmented skin cells that can appear anywhere on the body. They vary in color, shape, and size, and most are completely harmless. However, some moles may change over time due to sun exposure, hormonal changes, or genetic factors.
As a general rule in my practice, I advise patients to monitor any new or changing moles and to come in for evaluation if something doesn’t look or feel right.
Types of Moles:
- Congenital Moles – Present at birth and may grow over time.
- Common Moles – Typically small, round, and brown or tan in color.
- Atypical (Dysplastic) Moles – Irregular in shape, larger than normal, and can resemble melanoma.

Mole scanning procedure
When Should You Consider Mole Removal?
There are two primary reasons people choose to remove moles: medical concerns and cosmetic reasons.
Medical Reasons for Mole Removal:
✅ Asymmetry – One half of the mole doesn’t match the other.
✅ Border Irregularity – Edges are uneven, jagged, or blurred.
✅ Color Changes – Multiple shades of brown, black, red, or white.
✅ Diameter Growth – Larger than a pencil eraser (6mm).
✅ Evolving – Changes in size, shape, color, or texture over time.
These signs may indicate melanoma, a type of skin cancer. Early detection is crucial. If there’s ever any uncertainty, I perform a biopsy to ensure we’re not missing something serious.
Cosmetic Reasons for Mole Removal:
Even if a mole is harmless, it may be removed for aesthetic purposes or if it causes irritation (e.g., rubbing against clothing or jewelry). Many of my patients tell me that removing a bothersome mole gives them a boost in confidence—something I always support if the removal can be done safely.
Mole Removal Treatment Options
At Aesthetic Dermatology, we offer several safe and effective mole removal procedures based on the size, location, and type of mole. I always tailor the approach based on individual needs and skin type.
Mole removal procedure
1️⃣ Surgical Excision
The mole is carefully cut out, along with a small margin of surrounding skin.
Stitches may be needed, especially for larger moles.
Ideal for deeper or suspicious-looking moles.
2️⃣ Shave Removal
The mole is shaved off at the skin level using a scalpel.
No stitches are needed, and healing is usually quick.
Best for raised moles.
Aftercare & Healing

Before and after mole removal procedure
After mole removal, it’s important to follow proper aftercare guidelines to prevent infection and minimize scarring:
✔️ Keep the area clean.
✔️ Apply vaseline and cover with a bandage if needed.
✔️ Avoid picking at scabs.
✔️ Use sunscreen on the treated area to prevent darkening or discoloration.
In most cases, healing takes one to two weeks, depending on the treatment method. I personally follow up with patients when needed to ensure healing is progressing as expected.
Schedule a Skin Check Today!
Whether you’re concerned about a mole or simply want to remove one for cosmetic reasons, I’m here to help. My team and I at Aesthetic Dermatology are committed to providing expert skin evaluations and advanced treatment options in a caring and patient-focused environment.
If you have questions or would like a professional opinion on a mole, don’t hesitate to book a consultation. Your skin deserves attention and care—and we’re here to provide it.
Psoriasis Flare-Ups: How to Prevent and Treat Them

Psoriasis is a chronic autoimmune skin condition that causes red, scaly patches on the skin. While there is no cure, managing psoriasis effectively can help reduce flare-ups and keep symptoms under control. Whether you’re dealing with mild patches or severe breakouts, understanding what triggers psoriasis and how to treat it can make a significant difference in your quality of life. Visiting your board-certified dermatologist is always best to most effectively manage your psoriasis, but here are a few tips and tricks that all psoriasis patients should know.
What Causes Psoriasis Flare-Ups?

Psoriasis flares can be unpredictable, but certain triggers tend to worsen symptoms:
- Stress – One of the biggest culprits, stress can cause inflammation and trigger new outbreaks.
- Cold, Dry Weather – Winter months often bring drier skin, which can lead to increased scaling and irritation.
- Skin Injuries – Cuts, burns, bug bites, and even excessive scratching can lead to new psoriasis patches (a reaction known as the Koebner phenomenon).
- Infections – Illnesses like strep throat can trigger immune responses that cause flare-ups.
- Certain Medications – Some drugs, such as beta-blockers, lithium, and antimalarial medications, may worsen or even cause psoriasis.
- Alcohol & Smoking – Both have been linked to increased psoriasis severity and more frequent flares.
How to Prevent Psoriasis Flare-Ups
While psoriasis can’t be completely avoided, taking proactive steps can reduce the frequency and severity of flares:
- Moisturize Daily – Keeping your skin hydrated prevents cracking and irritation by strengthening your skin barrier. Look for thick creams, ointments, or lotions with ceramides, shea butter, or hyaluronic acid.
- Manage Stress – Meditation, yoga, and regular exercise can help keep stress levels in check.
- Avoid Harsh Soaps & Fragrances – Use gentle, fragrance-free skincare products to avoid irritation.
- Use a Humidifier – Adding moisture to the air, especially in winter, can prevent skin from drying out.
- Follow a Healthy Diet – While there is no specific diet that improves symptoms for all psoriasis patients, some find that anti-inflammatory foods like fatty fish, leafy greens, and nuts help may reduce symptoms.
Effective Treatments for Psoriasis

Treatment for psoriasis can be individualized depending on the severity, body parts affected, and previous treatments tried. Dermatologists offer a range of treatments to help control psoriasis and minimize discomfort:
1. Topical Treatments
- Corticosteroids – Reduce inflammation and itching for mild to moderate psoriasis.
- Vitamin D Analogs (Calcipotriene, Calcitriol) and other non-steroidal topicals – Slow skin cell growth to reduce scaling and decrease inflammation.
- Salicylic Acid & Coal Tar – Help soften and remove thick plaques.
2. Phototherapy (Light Therapy)
- Narrowband UVB Therapy – A safe, effective treatment that slows excessive skin cell growth.
- XTRAC Laser – an intense laser treatment specifically targeting psoraisis plaques that is appropriate for small areas of the body.
3. Systemic Treatments (For Moderate to Severe Cases)
- Biologic Medications – Injectables that target specific immune responses to prevent inflammation (e.g., Humira, Stelara, Cosentyx, Skyrizi).
- Oral Medications – Methotrexate, cyclosporine, and apremilast, among others can help control severe psoriasis.
When to See a Dermatologist

Dr Laura Schilling, a board-certified dermatologist
It can be beneficial to see a board-certified dermatologist at any stage and severity of psoriasis. This can ensure you have a proper diagnosis and optimized treatment plan. New advancements in psoriasis treatment have made it possible to live a comfortable, flare-free life. In addition, your dermatologist can discuss and help screen for any associated conditions such as psoriatic arthritis and cardiovascular problems, which psoriasis patients are at a higher risk for.
By understanding your triggers, following a skincare routine, and seeking medical guidance, you can keep psoriasis under control and reduce the impact it has on your daily life. Schedule an appointment with one of our dermatologists to find the best plan for your skin!
Don’t Let the Sun Strike You Out: Why Baseball Players and Fans Need Sunscreen

By: Dr. Jamie Altman, Board-Certified Dermatologist.
As a dermatologist and a lifelong baseball fan here in Pennsylvania, I’ve seen my fair share of sunburns, and I can tell you they don’t just happen at the beach. Whether you’re playing shortstop, coaching Little League, or sitting in the stands watching the Phillies, one thing remains the same: the sun is always in the game.
Baseball is one of the few sports that keeps players and fans out in direct sunlight for hours at a time, often during the sun’s peak intensity. Unlike hockey or basketball, where the action happens indoors, baseball offers little refuge from harmful UV rays. And in the stands? If you’re lucky enough to get a seat under the overhang, great, but for most fans, watching nine innings means baking in the sun. That’s why sunscreen isn’t just a good idea, it’s essential—not just for preventing burns, but also for maintaining healthy skin aesthetics in the long run.
The Hidden Dangers of a Day at the Ballpark

Pennsylvania may not be Florida or Arizona, but don’t let that fool you. UV rays are still strong here, even on cloudy or cooler days. In fact, up to 80% of UV radiation can penetrate clouds, meaning overcast days aren’t as protective as you might think. And while it’s easy to notice a sunburn after an afternoon game, the real concern is long-term: cumulative sun exposure leads to premature aging, sunspots, and, most critically, skin cancer, including melanoma, the deadliest form.
I see it all the time—patients who think they’re only at risk when they lay out in the sun. But a few baseball games each summer, a season of coaching, or a childhood spent playing Little League without protection all add up over time. Protecting your skin isn’t just about health; it’s also about preserving a skin care aesthetic that keeps your skin looking youthful and damage-free for years to come.
Sunscreen: Your Best Defensive Play
So, how do you protect yourself without missing a pitch? Here’s the game plan:
1. Pick the Right Sunscreen
- Use a broad-spectrum sunscreen with SPF 30 or higher to shield against both UVA and UVB rays.
- If you’ll be sweating (which, let’s be honest, you will), opt for a water-resistant formula.
- Chemical sunscreens are generally considered safe. However, zinc and titanium-based sunscreens are great mineral-based options.
2. Apply Enough – And Then Some
- Most people under-apply sunscreen. You need about a shot glass full (one ounce) to cover exposed areas properly.
- Don’t forget easy-to-miss spots like your ears, the back of your neck, and the tops of your feet.
3. Reapply Like a Pro
- Sunscreen isn’t a one-and-done deal. Reapply every two hours, or sooner if you’re sweating a lot.
4. Don’t Just Rely on Sunscreen
- A baseball cap helps, but it doesn’t protect your ears or the sides of your face. A wide-brimmed hat is even better.
- Wear sunglasses to protect your eyes from UV damage.
- And if you’re watching a game, try to sit in a shaded area for extra coverage.

Bottom Line: Protect Yourself and Play Smart
Baseball is a game of strategy, and sun protection should be part of yours. Whether you’re stepping up to the plate or sitting back with a hot dog in the stands, don’t let the sun get the best of you. Keeping your skin safe from UV damage not only lowers your risk of skin cancer but also helps you maintain a skin aesthetic that reflects health and care.
So, before you head out to your next game, grab your sunscreen, throw on a hat, and stay protected—because no one wants to leave the ballpark with a sunburn as their souvenir. Protect your skin today so it stays healthy and radiant for seasons to come!
Stay sun-safe, and enjoy the game!
Overcoming the Fear of Cosmetic Treatments

Hi, I’m Dr. Laura Schilling, and today I want to talk about something I hear all the time: the hesitation, or even fear, of trying cosmetic treatments like Botox, Dermaplaning, or Microneedling. Many people are curious about these treatments but worry about pain, downtime, or unnatural results. This is especially true for those considering Vivace microneedling, one of the most advanced skin-rejuvenation treatments available today.
The good news? These treatments are far less intimidating than you might think. Whether you’re interested in traditional microneedling or Vivace RF microneedling, both options are safe, minimally invasive, and highly effective for boosting collagen, tightening skin, and improving texture. Let’s break it down so you can feel confident in making the right choice for your skin.
Why You Don’t Need to Worry

The most important thing to know is that these treatments are designed to be safe, gentle, and effective. They don’t require surgery, they have little to no downtime, and they’re performed in your board-certified dermatologist’s office by professionals who specialize in enhancing—not changing—your natural beauty.
Microneedling: Your Skin’s Natural Collagen Booster
Microneedling might sound intimidating—after all, the word “needle” is in the name—but in reality, it’s a gentle way to stimulate your skin’s own healing powers. It involves using tiny, fine needles to create micro-injuries on the skin’s surface. This kickstarts your body’s natural collagen and elastin production, which helps to smooth out fine lines, improve texture, and even fade acne scars over time.
What makes microneedling so great?
✔️ It’s not as scary as it sounds—the needles are incredibly fine, and a numbing cream is used so there’s little to no discomfort.
✔️ The results develop naturally—your skin repairs itself gradually, leading to a fresher, healthier look.
✔️ There’s minimal downtime—you might have some redness for a day or two, but that’s about it.
If you want long-term improvement in your skin’s texture and firmness without invasive procedures, microneedling is one of the best options available.
What Is Vivace Microneedling?
For those looking for an advanced, next-level microneedling treatment, Vivace RF Microneedling is a top choice. This treatment combines traditional microneedling with radiofrequency (RF) energy and LED light therapy to provide even greater skin-tightening and rejuvenation benefits.
Vivace Microneedling Benefits
✔️ Tightens and firms the skin – The addition of radiofrequency energy stimulates deeper layers of collagen production, making it ideal for firming sagging skin.
✔️ Minimizes fine lines and wrinkles – By boosting natural collagen and elastin, Vivace microneedling helps smooth out early signs of aging.
✔️ Reduces acne scars and uneven texture – The microneedling process helps break down scar tissue, leading to clearer, smoother skin over time.
✔️ Less downtime compared to traditional microneedling – The advanced design of the Vivace system ensures a more comfortable experience and faster recovery.
✔️ Safe for all skin types – Unlike some laser treatments, Vivace RF microneedling is safe for all skin tones. Furthermore, with appropriate aftercare, treatments can be performed throughout the entire year, including summer months.
If you’re searching for the best microneedling treatment with extra skin-tightening benefits, Vivace RF Microneedling is a high-tech solution that delivers incredible results with minimal discomfort.
Botox: A More Rested, Refreshed You
When people hear “Botox,” their first thought is often of overdone celebrity faces that look frozen or unnatural. But in reality, Botox is simply a way to soften lines and prevent new ones from forming—not to erase your expressions.
Here’s what you need to know:
✔️ Botox doesn’t freeze your face—when done correctly, it just smooths out wrinkles while letting you keep natural movement.
✔️ The results look natural—the goal is to enhance, not transform, your look.
✔️ Treatments are customized to your needs – Botox should not be a cookie cutter approach; injections can be tailored to your concerns and your anatomy.
The key is working with a board-certified dermatologist who knows how to apply Botox in a way that enhances your natural beauty. The best results make you look like yourself—just a little fresher and more well-rested. It can truly be your little secret!
Still Nervous? Here’s What You Can Do
If you’re on the fence about trying a cosmetic treatment, the best thing you can do is ask questions. A consultation with your board-certified dermatologist can help ease concerns by explaining exactly what to expect and ensuring you’re comfortable before starting any procedure.
Here are some ways to ease any lingering doubts:
✔️ Start small – If you’re curious but nervous, try a minimally invasive treatment first. Many options have little to no downtime.
✔️ Ask for before-and-after photos – Seeing real results from actual patients can help set realistic expectations.
✔️ Choose a certified provider with strong credentials – Look for someone with experience, patient testimonials, and a consultation process that makes you feel at ease.
Final Thoughts: Is Vivace Microneedling Right for You?
At the end of the day, cosmetic treatments aren’t about changing who you are. They’re about feeling confident in your own skin. Whether you want smoother skin, a subtle boost in collagen production, or a refreshed look, these treatments offer simple, effective solutions that don’t require major commitments or recovery time.
If you’re especially interested in improving skin firmness, reducing wrinkles, and enhancing collagen production, Vivace RF microneedling is one of the best choices available today. This advanced microneedling technology provides noticeable, long-lasting results with minimal downtime and maximum benefits.
Still have questions? Reach out to your board-certified dermatologist’s office for a consultation – in Media and Paoli, PA. You might just find that these treatments are much easier – and more rewarding – than you ever imagined.

Why Preventative Botox Is Becoming a Popular Choice Among Younger Adults
Botox has long been associated with smoothing out wrinkles, but in recent years, it has taken on a new role: prevention. More people in their 20s and early 30s are opting for “preventative Botox” to slow down signs of aging before they even appear. What’s driving this shift, and does starting early actually make a difference?
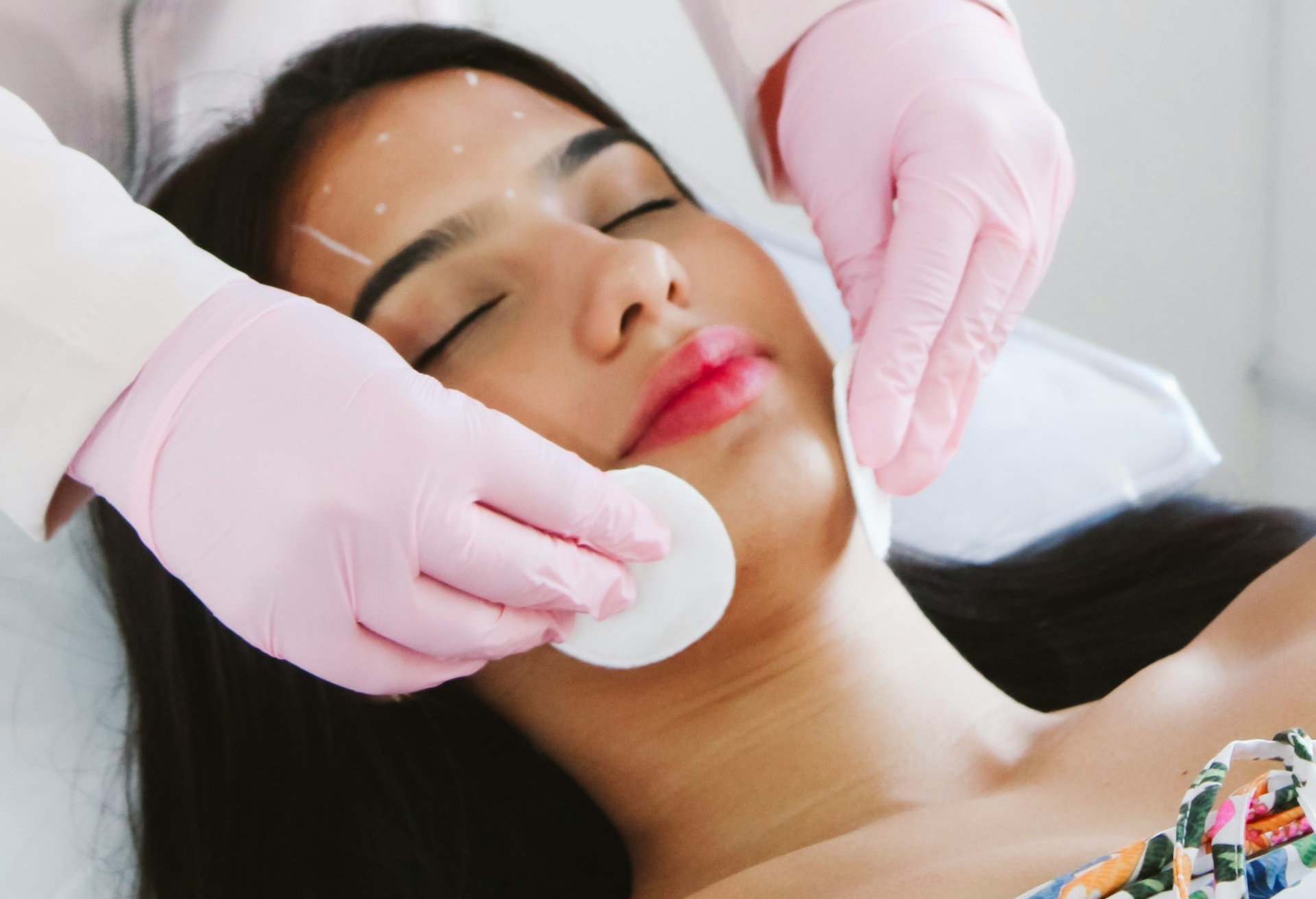
What Is Preventative Botox?
Preventative Botox is different from traditional Botox in that it’s used before wrinkles become deeply etched into the skin. The treatment involves injecting small amounts of botulinum toxin into areas that tend to develop fine lines, such as the forehead, between the brows, and around the eyes.
The goal is to reduce repetitive facial movements—like frowning, squinting, or raising the eyebrows—that gradually cause lines to form. Instead of erasing existing wrinkles, preventative Botox helps delay their development, keeping the skin looking smoother for longer.
Why Are Younger Adults Turning to Botox Sooner?
Several factors are fueling the trend of early Botox use:
-
Social Media’s Influence – With platforms like Instagram and TikTok constantly showcasing beauty trends, non-invasive treatments like Botox are becoming more common among young adults. The normalization of cosmetic procedures has made early Botox a common topic among beauty-conscious individuals.
-
A Shift in Skincare Awareness – Today’s younger generations have greater access to expert advice than ever before. Dermatologists, beauty bloggers, and skincare specialists regularly discuss the benefits of early intervention when it comes to aging. As a result, Botox is now often viewed as part of a proactive skincare routine rather than a last-minute fix.
-
More Subtle, Natural-Looking Results – Advances in cosmetic techniques have made Botox treatments more refined than they used to be. The goal is no longer to freeze facial expressions but to maintain a youthful, refreshed look while keeping natural movement intact.
The Benefits of Starting Botox Early
One major advantage of preventative Botox is that it may help reduce the need for more intensive treatments later on. By addressing fine lines before they fully develop, many patients find they require fewer injections over time, making it a long-term investment in their appearance.
Convenience is another factor. Botox appointments are quick, with little to no recovery time, making them easy to fit into a busy lifestyle. For many, the treatment feels like an extension of their usual skincare routine, much like using anti-aging serums or getting regular facials.
What to Consider Before Getting Preventative Botox
While preventative Botox has its advantages, it’s not for everyone. Consulting with a qualified dermatologist or aesthetic provider is essential to determine if it’s the right approach based on skin type, facial structure, and overall goals.
Experts also emphasize the importance of moderation. Too much Botox at an early age can weaken facial muscles unnecessarily, which may affect natural expressions over time. Finding a skilled injector who understands how to create a subtle, balanced look is key to achieving the best results.
Final Thoughts
The rise of preventative Botox reflects a shift in how younger generations approach aging. Instead of waiting for wrinkles to appear, more people are taking early action to maintain their skin’s smooth, youthful appearance. While Botox isn’t a necessity for everyone, those who choose to start early see it as a strategic way to age gracefully while preserving their natural look.
Visit Our Locations
Media, PA
| Mon: | 7:30 am - 5:30 pm |
| Tue: | 8:00 am - 4:00 pm |
| Wed: | 7:30 am - 4:00 pm |
| Thu: | 7:30 am - 4:00 pm |
| Fri: | 7:30 am - 1:00 pm |
Paoli, PA
| Mon: | 8:00 AM - 4:30 PM |
| Tue: | 8:00 AM - 4:00 PM |
| Wed: | 8:00 AM - 5:30 PM |
| Thu: | 8:00 AM - 4:30 PM |
| Fri: | 8:00 AM - 5:00 PM |
Stay Informed with our Newsletter

Book Your Appointment Today!
Choose the option that works best for you:
Prefer to speak with someone? Call or text us:

Media, PA Office - Call or Text (610) 566-7300

Paoli, PA Office - Call or Text (610) 647-4161
Want to book online now? Select a provider below:
Note: Self-scheduling is currently available for Dr. Ko & Bridget Lolli. For all other providers, please call or text the office.