Medical Dermatology in Paoli, PA: What to Expect at a Board-Certified Dermatology Practice
If you’ve been searching for a dermatologist in Paoli, PA — or looking for dermatology care serving Malvern, Wayne, Berwyn, Exton, or West Chester — you may already know that not all dermatology practices offer the same scope of care. Some focus primarily on cosmetics. Others handle only routine skin checks. A full-service medical dermatology practice does something more: it treats the conditions that affect your skin’s health, function, and long-term wellbeing.

At Aesthetic Dermatology Associates in Paoli, our board-certified dermatologists and clinical team provide comprehensive medical dermatology care for patients throughout Chester County and the Main Line. This article walks through what that looks like in practice — what conditions we treat, how we approach them, and what to expect as a patient.
What Is Medical Dermatology?
Medical dermatology refers to the diagnosis and treatment of skin conditions that have a clinical, not purely cosmetic, basis. This includes everything from chronic conditions like eczema and psoriasis to acute concerns like acne, to serious diagnoses like skin cancer.
While cosmetic dermatology addresses how the skin looks, medical dermatology addresses how the skin functions — its barrier integrity, its immune response, its susceptibility to disease. The two often overlap: a patient being treated for skin cancer may also have cosmetic concerns about scarring; a patient managing psoriasis may struggle with self-confidence. Good dermatological care acknowledges the whole picture.
Conditions We Treat at Our Paoli Office
Skin Cancer
Skin cancer is the most common type of cancer in the United States — and one of the most treatable, when caught early. At Aesthetic Dermatology Associates, skin cancer care begins with thorough full-body skin exams to identify suspicious lesions, followed by biopsy when indicated and a treatment plan tailored to the type and stage of cancer.
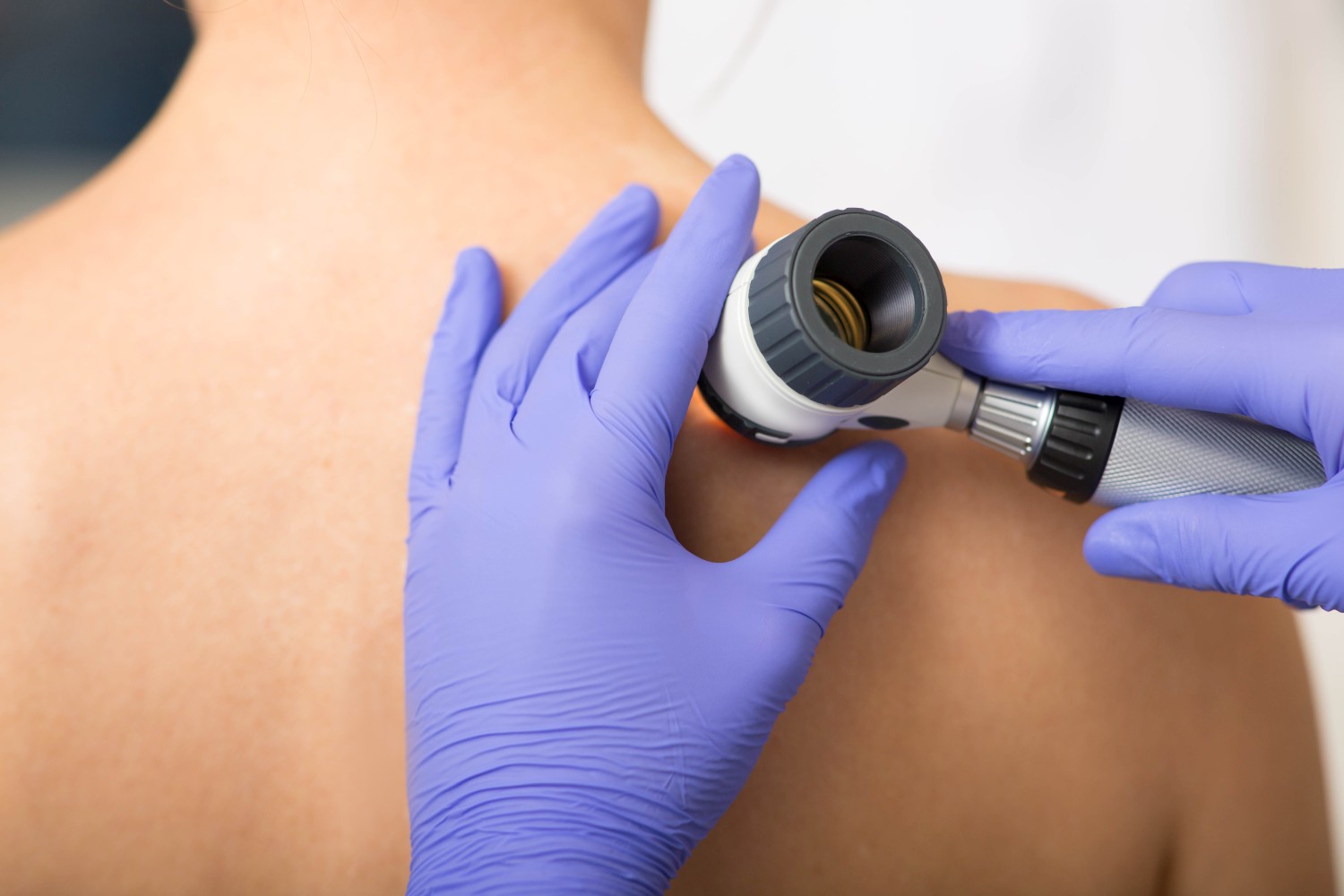
The most common types we diagnose and treat are basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). Melanoma, while less common, is the most serious form and requires prompt attention when detected.
For patients throughout the Paoli and Main Line area, early detection is everything. If you haven’t had a full-body skin exam recently — particularly if you’ve had significant sun exposure over your lifetime, a family history of skin cancer, or a personal history of sunburns — scheduling a screening is one of the most impactful things you can do for your long-term health.
Photodynamic Therapy (PDT)
Photodynamic Therapy is a light-activated treatment that targets sun-damaged and precancerous skin while protecting surrounding healthy tissue. It’s one of the most effective non-surgical options for treating actinic keratoses — the rough, scaly patches that develop after years of UV exposure and can progress to squamous cell carcinoma if left untreated.
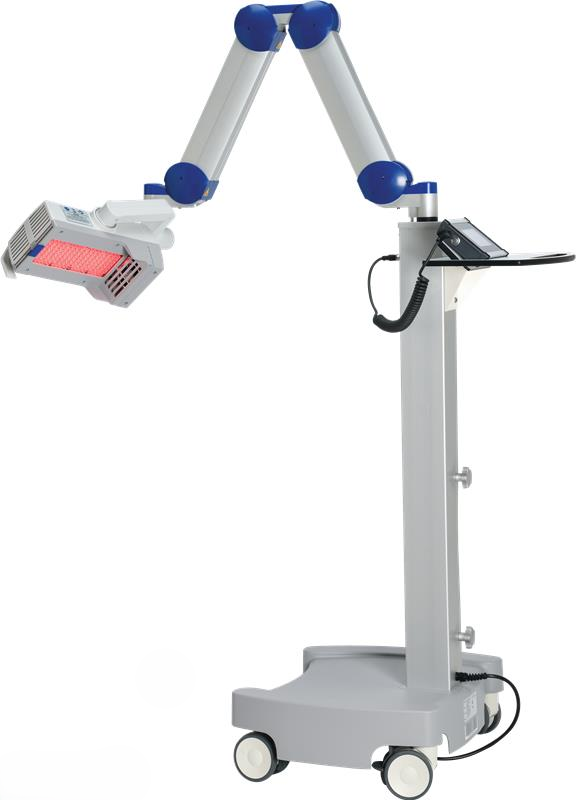
Image: PDT Device used in our clinics
The treatment involves applying a photosensitizing agent to the skin, allowing it to absorb into abnormal cells, then activating it with a specific wavelength of light. The result is targeted destruction of damaged cells with minimal impact on healthy surrounding tissue.
PDT is particularly well-suited for patients with widespread sun damage across the face, scalp, or forearms — areas where treating each lesion individually would be impractical. It also offers a cosmetic benefit: many patients notice an improvement in overall skin tone and texture following treatment.
For patients coming from Malvern, Berwyn, Wayne, and surrounding areas, PDT is available at our Paoli office without the need for hospital visits or surgical settings.
Dermatologic Surgery
When a skin lesion needs to be removed — whether a concerning mole, a cyst, a skin cancer, or a growth causing discomfort — dermatologic surgery provides a precise, effective solution. All surgical procedures at our Paoli practice are performed comfortably in our office with local anesthesia, so you can return home the same day.
There’s no need for a hospital, a surgical center, or general anesthesia. Most patients describe the procedure itself as far less intimidating than they expected — the local anesthetic does its work, and the process is straightforward.
Common dermatologic surgeries we perform include excision of skin cancers, removal of cysts and lipomas, and treatment of other growths that require histopathological evaluation. Each specimen removed is sent for pathology analysis to confirm complete removal and accurate diagnosis.
For patients in Exton, West Chester, and across Chester County who’ve been referred for a procedure, our office offers a calm, clinical environment close to home.
Acne Treatment
Acne is one of the most common skin conditions we treat — and one of the most misunderstood. It’s not a teenage problem that resolves on its own, and it’s not simply a matter of better skincare. Acne is a medical condition with multiple contributing factors: excess sebum production, bacterial overgrowth, inflammation, hormonal influence, and genetics all play a role.

At Aesthetic Dermatology Associates, we provide evidence-based treatments to manage and reduce acne effectively — not just manage outbreaks as they occur, but address the underlying drivers. That may include topical or oral prescription medications, hormonal therapy where appropriate, in-office procedures, or a combination.
We also take scarring seriously. Acne that’s inadequately treated — or that’s been present for years — can leave lasting marks. Addressing active acne early, aggressively, and correctly is the best way to protect the skin’s long-term appearance and health.
Patients searching for a dermatologist in Paoli or Malvern for acne care will find that we approach this condition with the same clinical seriousness we bring to any other diagnosis.
Eczema
Eczema — or atopic dermatitis — is a chronic, non-contagious condition that causes dry, itchy, and inflamed skin. It’s particularly common in children, but it affects patients of all ages, and many adults live with eczema for decades without receiving adequate treatment.
The condition is driven by a compromised skin barrier that allows moisture to escape and irritants to penetrate. This triggers an immune response that causes the characteristic redness, itching, and flaking. In moderate to severe cases, it can significantly affect sleep, concentration, and quality of life.
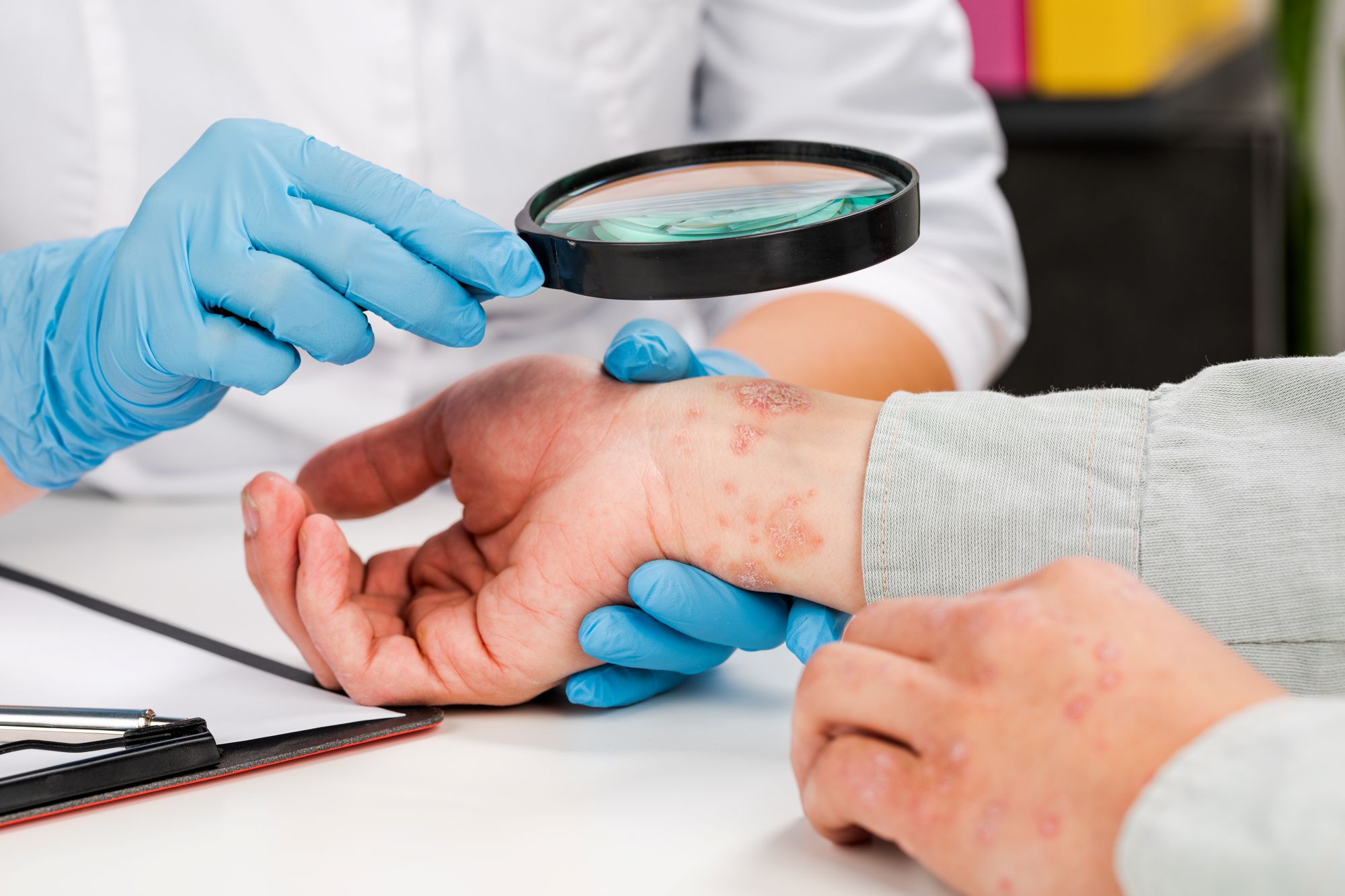
Effective eczema management involves more than a hydrocortisone cream. Our approach addresses the skin barrier directly — with appropriate moisturization protocols, trigger identification, and prescription treatments that range from topical corticosteroids and calcineurin inhibitors to newer targeted biologics for patients with moderate to severe disease.
For families in Wayne, Berwyn, and surrounding communities looking for a dermatologist who will take a chronic eczema diagnosis seriously rather than issue a repeat prescription, our Paoli office offers the continuity of care this condition requires.
Psoriasis
Psoriasis is a chronic autoimmune skin condition characterized by itchy, scaly patches that most commonly appear on the torso, elbows, knees, and scalp. Beyond the visible symptoms, psoriasis can impact sleep, focus, and overall comfort — and is associated with systemic inflammation that carries implications beyond the skin, including increased cardiovascular risk and a condition called psoriatic arthritis.
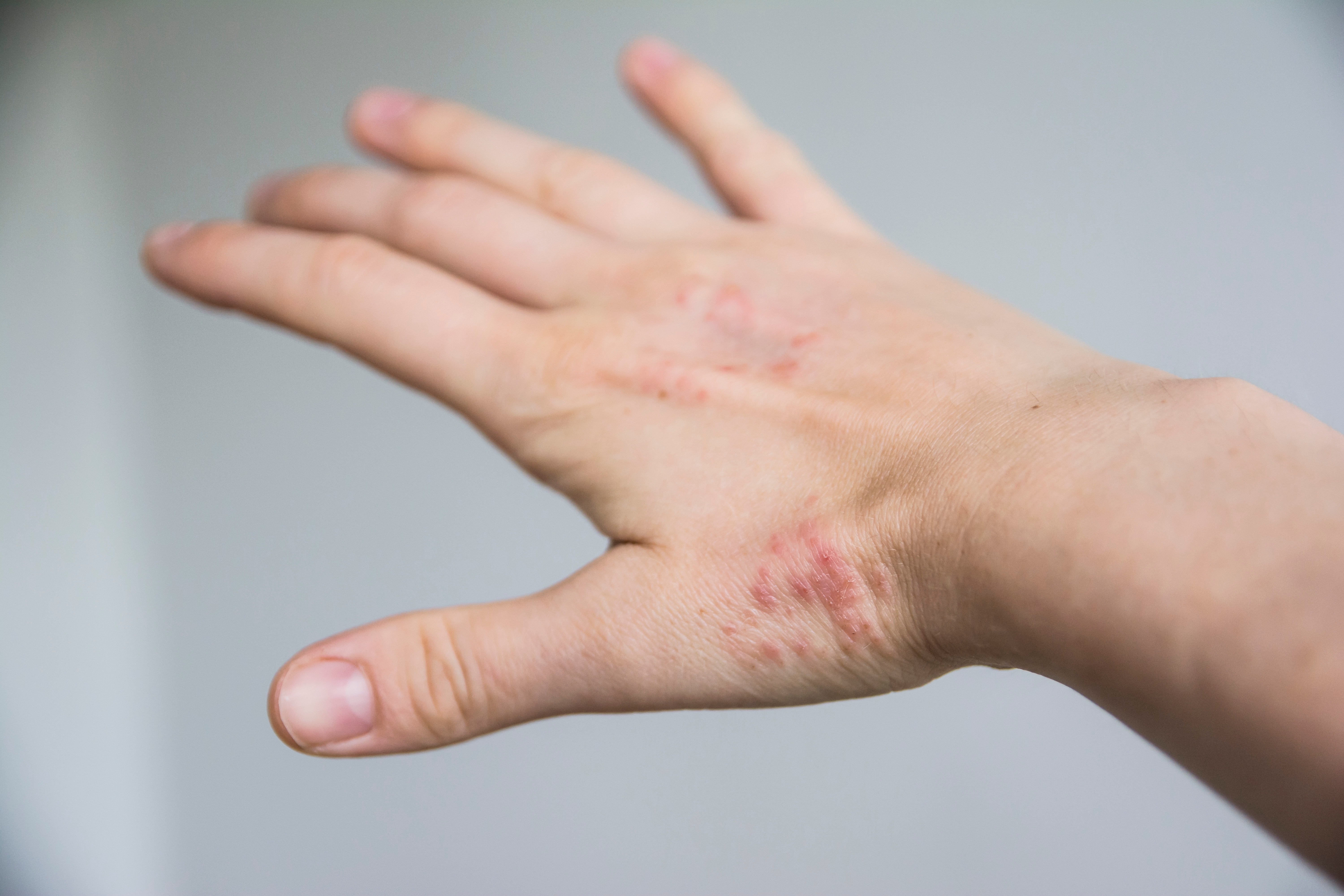
This is a condition that benefits significantly from specialist management. General practitioners can offer basic treatment, but a board-certified dermatologist brings a broader range of treatment options — including topical therapies, phototherapy, oral systemic medications, and biologics that have transformed outcomes for moderate to severe psoriasis patients over the past decade.
If you’ve been managing psoriasis on your own, or if previous treatment hasn’t given you adequate control, a consultation at our Paoli office is a practical next step. We serve psoriasis patients from across the Main Line, including Malvern, Exton, and West Chester.
Mole Removal and Evaluation
Moles are pigmented cell clusters that vary in size, shape, and color — most are entirely harmless and require no intervention. But changes in a mole’s appearance deserve medical attention. The classic warning signs follow the ABCDE framework: Asymmetry, Border irregularity, Color variation, Diameter greater than 6mm, and Evolution over time.
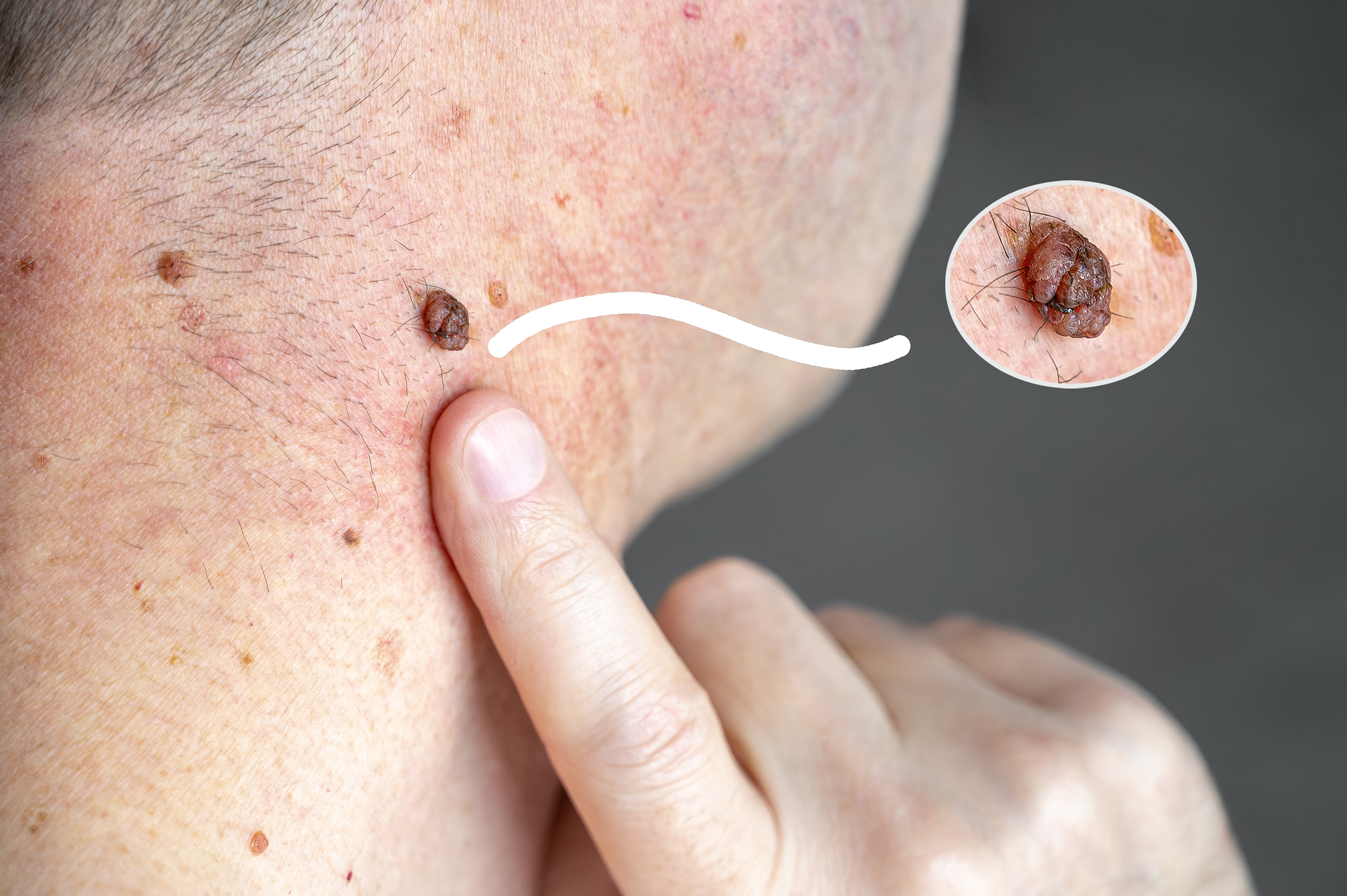
If you’ve noticed a mole changing, itching, bleeding, or simply looking different than it did before, the appropriate first step is a clinical evaluation — not a wait-and-see approach.
At Aesthetic Dermatology Associates, mole evaluation is part of routine full-body skin exams. When a mole warrants removal — either for diagnostic purposes or because it’s causing concern — we perform the procedure in-office with minimal discomfort and send all specimens to pathology.
Why See a Dermatologist?
Many skin conditions are best managed by a board-certified dermatologist. Dermatologists complete four years of residency training specifically focused on the skin, hair, nails, and mucous membranes, plus any additional fellowship training. They have the clinical experience to identify conditions that may look similar on the surface but require very different treatment approaches.
For patients in Paoli, Malvern, Wayne, Berwyn, Exton, and West Chester, having a board-certified dermatologist accessible on the Main Line — rather than requiring a trip into Philadelphia — makes regular skin care practical rather than something that gets postponed indefinitely.
What to Expect at Your First Appointment
New patients at Aesthetic Dermatology Associates are seen for a thorough consultation. Depending on your concerns, this may include a full-body skin exam, evaluation of specific lesions or conditions you’ve noticed, a review of your skin and family history, and a discussion of treatment options.
We don’t rush appointments. Medical dermatology requires clinical judgment, and clinical judgment requires time — to look carefully, to ask the right questions, and to explain findings in a way that makes sense to you.
If you’re coming to us from Paoli, Malvern, Wayne, Berwyn, Exton, West Chester, or anywhere across Chester County and the Main Line, you’re welcome to request an appointment online or call our office directly.
How to Perform a Skin Cancer Self-Exam: What Dermatologists Look For
Featuring Dr. Clare Goggins, a board-certified dermatologist providing expert medical care to both adult and pediatric patients.
You’ve noticed something on your skin that wasn’t there before. Or maybe there’s a mole that looks different than it used to. So you’re doing what most people do at 11 PM on a Tuesday: searching the internet, comparing what you’re seeing to images online, and quietly spiraling into worst-case scenarios.
If you’re here because you’re worried about skin cancer, let’s start with this: noticing changes in your skin and taking them seriously is exactly what you should be doing. Skin awareness isn’t paranoia—it’s smart healthcare.
Dr. Clare Goggins, a board-certified dermatologist at Aesthetic Dermatology Associates, sees patients every week who are anxious about skin changes they’ve discovered. Her approach combines Johns Hopkins-trained clinical expertise with something equally important: helping patients understand what they are actually looking at.
“The goal of self-examination isn’t to diagnose yourself,” Dr. Goggins explains. “It’s to become familiar enough with your own skin that you notice when something changes. That awareness—combined with regular professional screenings—is what catches skin cancer early, when it’s most treatable.”
Why Self-Exams Matter (But Can’t Replace Your Dermatologist)

Here’s something that might surprise you: most skin cancers are first noticed by patients themselves, not by doctors during routine exams. You see your skin every single day. Your dermatologist sees it once, maybe twice, a year depending on your medical history.
But here’s the critical distinction: self-exams help you know when to see a doctor. They don’t tell you what something is or isn’t. That anxiety you’re feeling while comparing your mole to images online? That’s your cue to stop searching and schedule an appointment instead.
The ABCDE Method: What Dermatologists Look For
Dermatologists recommend a framework called the ABCDE method to identify suspicious moles and melanoma. This is the same clinical approach Dr. Goggins uses when examining patients.
Asymmetry: If you drew a line through the middle of the mole, would both halves look the same? Normal moles are typically symmetrical. Melanomas often aren’t.
Border irregularity: Normal moles have smooth, even edges. If the border is ragged, notched, blurred, or irregular, that’s worth noting.
Color variation: A normal mole is usually one uniform color. If you’re seeing multiple colors within the same spot (brown mixed with black, red, white, or blue), that’s a warning sign.
Diameter: Melanomas are often (though not always) larger than 6mm—about the size of a pencil eraser. But don’t discount something just because it’s small.
Evolving: This is the most important letter. Has the mole changed over the past few weeks or months? Is it getting bigger, darker, raised, or behaving differently? Change over time is the single biggest red flag.
Dr. Goggins adds an important caveat: “The ABCDE method is incredibly useful, but it’s not foolproof. That’s why the ‘ugly duckling’ sign matters too—if you have one mole that just looks different from all your other moles, even if it doesn’t check the ABCDE boxes, call your dermatologist to have it examined.”
How to Perform a Self-Exam (Step by Step)
You don’t need special equipment or medical training. You need decent lighting, two mirrors (a full-length mirror and a handheld one), and about 15 minutes of uninterrupted time. Do this once a month.
Start at your face and scalp. Examine your face, ears, neck, and scalp carefully. Use the handheld mirror to check areas you can’t see directly. If you have thick hair, use a blow dryer to part sections so you can see your scalp.
Move down your body systematically. Check your shoulders, chest, and torso—front and back. Look under your arms. Examine both sides of your arms, your hands, between your fingers, and under your nails.
Check areas that don’t see the sun. Look at your buttocks, genital area, and the backs of your legs using your mirrors. Melanoma doesn’t only develop on sun-exposed skin—it can appear anywhere.
Don’t skip your feet. Check the tops, bottoms, between your toes, and your toenails.
Optional but useful: Take photos. If you have a lot of moles or spots you’re monitoring, taking monthly photos can help you track changes over time more objectively than memory alone.
What To Look For: Warning Signs vs. Normal Findings

Things that usually warrant a call to your dermatologist:
- A new growth appearing after age 30, especially one that’s growing or changing
- Any mole that looks noticeably different from your other moles (the ugly duckling sign)
- A sore that doesn’t heal within 3-4 weeks
- A spot that repeatedly itches, bleeds, crusts over, or oozes
- A mole that’s changing in size, shape, color, or texture
- A dark streak appearing on a fingernail or toenail
Common benign findings that may catch your attention:
Seborrheic keratoses look like brown or black growths stuck onto the skin’s surface. They’re extremely common as you age and can look concerning because they’re often dark and crusty, but they’re harmless.
Cherry angiomas are small, bright red bumps that appear with age. They’re clusters of blood vessels and are completely benign.
Skin tags are small, pedunculated pieces of extra skin. Annoying, yes. Dangerous, no.
Understanding the Three Main Types of Skin Cancer
Basal Cell Carcinoma (BCC)
This is the most common form of skin cancer. It can appear as a shiny pink bump, a scaly pink or red patch, or a pimple that won’t go away or sore that won’t heal. BCC grows slowly and rarely spreads beyond the skin. It is the least dangerous of the three main types of skin cancer, but it still needs to be treated. Treatment is usually straightforward—often a simple in-office procedure. Prognosis is excellent when caught early.
Squamous Cell Carcinoma (SCC)
SCC often appears as a firm, red nodule or a sharply demarcated, red, scaly patch. It can develop in old scars or chronic wounds. SCC is more aggressive than BCC and has a higher risk of spreading if left untreated. Like BCC, it’s highly treatable when caught early, typically with surgical removal or other in-office procedures.
Melanoma
Melanoma is the most serious of the three main types of skin cancer. It can develop within an existing mole or appear as a new dark spot on the skin. The ABCDE signs are particularly relevant for melanoma.
Melanoma can appear anywhere—on sun-exposed skin, but also in places like the soles of your feet, within nails, or even inside your mouth.
Here’s the crucial thing: melanoma caught at its earliest stage (melanoma in situ) is highly curable and there is very little risk for recurrence or metastatic spread. This information should motivate you to pay attention, not to panic.
What Happens If You Find Something Concerning
Make the appointment. Call your dermatologist’s office and be specific about what you’re seeing. Phrases like “I have a mole that’s changed” or “I have a sore that won’t heal” signal that you need to be seen relatively soon.
Dr. Goggins and her team at Aesthetic Dermatology Associates in Media and Paoli, PA, understand that the anxiety waiting to get in for the initial appointment is real. “We make every effort to see patients with concerning skin changes promptly,” she notes.
What to expect during your skin cancer screening:
Your dermatologist will perform a full-body skin examination. They’ll use a dermatoscope—a specialized magnification tool—to examine any spots that look suspicious. This is completely painless.
If something looks concerning, the only way to know definitively what it is involves a skin biopsy.
If a Skin Biopsy Is Recommended: What You Need to Know
A skin biopsy sounds scarier than it actually is. It’s a quick in-office procedure, done under local anesthetic, where a small sample of the suspicious tissue is removed and sent to a lab for analysis.
There are different types of biopsies:
- Shave biopsy: The lesion is shaved off at the level of the surrounding skin
- Punch biopsy: A small circular tool removes a deeper core of tissue
- Excisional biopsy: The entire lesion is removed along with a margin of surrounding skin
The procedure itself takes just minutes. You’ll feel the numbing injection (a brief pinch), and then you won’t feel the actual biopsy. Most people are surprised by how quick and straightforward it is.
How long do skin biopsy results take?
Most biopsy results are received within 7-10 business days. Feeling anxious while waiting for your biopsy results is understandable. The team at Aesthetic Dermatology Associates will be in touch as soon as we receive your results and will let you know the next steps, if any are needed.
What happens after a skin biopsy?
If the biopsy shows skin cancer, your dermatologist will discuss the specific type, the appropriate treatment options, and the next steps.
The important thing to remember: most skin cancers are highly treatable, especially when caught early.
Treatment Options When It Is Skin Cancer
For basal cell carcinoma and squamous cell carcinoma, treatment often involves surgical removal of the cancerous tissue—sometimes through standard excision, sometimes through Mohs surgery that removes cancer layer by layer while preserving healthy tissue. Other options can include topical treatments, cryotherapy, electrodessication & curretage, or radiation in specific cases.
For melanoma, treatment depends on the stage. Early-stage melanoma may only require surgical excision. More advanced cases might involve additional treatments including lymph node dissection, immunotherapy, targeted therapy, chemotherapy, and/or radiation.
Dr. Goggins emphasizes the collaborative nature of treatment planning: “Every patient’s situation is different. My job is to walk through the options, explain what each involves, and help patients make informed decisions about their care.”
Follow-up care after treatment typically involves regular skin checks to monitor for recurrence or new skin cancers.
Moving From Anxiety to Action
If you’ve found something on your skin that’s worrying you, the anxiety is understandable. But here’s what matters: you noticed. You’re paying attention. And that awareness is precisely what leads to early detection and successful treatment.
Regular self-exams combined with annual professional skin cancer screenings are the most effective strategy for catching skin cancer early. Self-exams help you develop a baseline understanding of your skin so you can spot changes. Professional screenings catch things you might miss.
The best thing you can do right now isn’t to keep searching the internet. It’s to schedule an appointment if you’ve noticed something that fits the warning signs.
Dr. Goggins’ Perspective: Empowerment Through Education
Dr. Clare Goggins completed her dermatology residency at Johns Hopkins, where she was selected as chief resident—a distinction that reflects both clinical excellence and dedication to teaching. She now applies that expertise to patients of all ages at Aesthetic Dermatology Associates.
“I want my patients to feel empowered, not scared,” Dr. Goggins explains. “Learning how to examine your own skin and knowing what to look for isn’t about creating anxiety—it’s about giving you the tools to take charge of your health. When patients come in because they noticed something concerning, I’m grateful. That vigilance saves lives.”
Her advice is direct: “If you’re looking at a spot on your skin and you can’t stop thinking about it, that’s your body telling you to get it checked out. Trust that instinct. Even if it turns out to be nothing, you’ll have peace of mind. And if it is something, we’ll handle it together.”
When in Doubt, Get It Checked Out
Skin cancer is one of the most common cancers, but it’s also one of the most treatable when caught early. The combination of monthly self-exams and annual dermatologist visits creates a safety net that catches problems while they’re still manageable.
If you’ve noticed a suspicious spot, if you have a mole that’s changed, if you have a sore that won’t heal—don’t wait. Aesthetic Dermatology Associates serves patients in Media and Paoli, PA, and Dr. Goggins sees both adult and pediatric patients.
The appointment you’re nervous about making? That’s the one that might save your life.
You’re not overreacting. You’re not wasting anyone’s time. You’re doing exactly what you should be doing: taking your health seriously.
Ready to schedule a skin cancer screening or discuss a concerning spot?
Dr. Goggins and her team are here to provide expert evaluation, clear answers, and compassionate care. Because when it comes to skin cancer, early detection isn’t just important—it’s everything.
Related links
See Dr. Goggins’ provider’s page on our website: https://adaderm.com/providers/clare-goggins-md/
Review 5-star rating given by patients on Zocdoc: https://www.zocdoc.com/doctor/clare-goggins-md-504595
Is Preventive Botox Real? A Skeptic’s Guide to What the Science Actually Says
So you’ve been thinking about Botox. Maybe a friend mentioned she started getting it, or you noticed a few lines showing up in photos that weren’t there a couple years ago. Or maybe you’re just curious whether all this “preventive Botox” talk is actually legit or just another way to get people spending money earlier.
Honestly, that’s a fair question to ask.
First, Some Things About Botox That Might Surprise You
Botox has been around since the late 1980s—not as a cosmetic treatment, but as a medical one. It was originally FDA-approved to treat crossed eyes and uncontrollable blinking. Doctors noticed something interesting: patients kept coming back saying their forehead lines had softened. The cosmetic application was essentially discovered by accident.
Today, Botox is used to treat chronic migraines, excessive sweating, overactive bladder, and even depression (there’s ongoing research suggesting that relaxing frown muscles may actually improve mood—the facial feedback hypothesis in action). The cosmetic use that everyone knows about? That came later, and it’s actually one of the most well-studied cosmetic procedures in existence.
Over 100 million vials have been sold worldwide since its approval. The safety profile at this point is extremely well-documented.
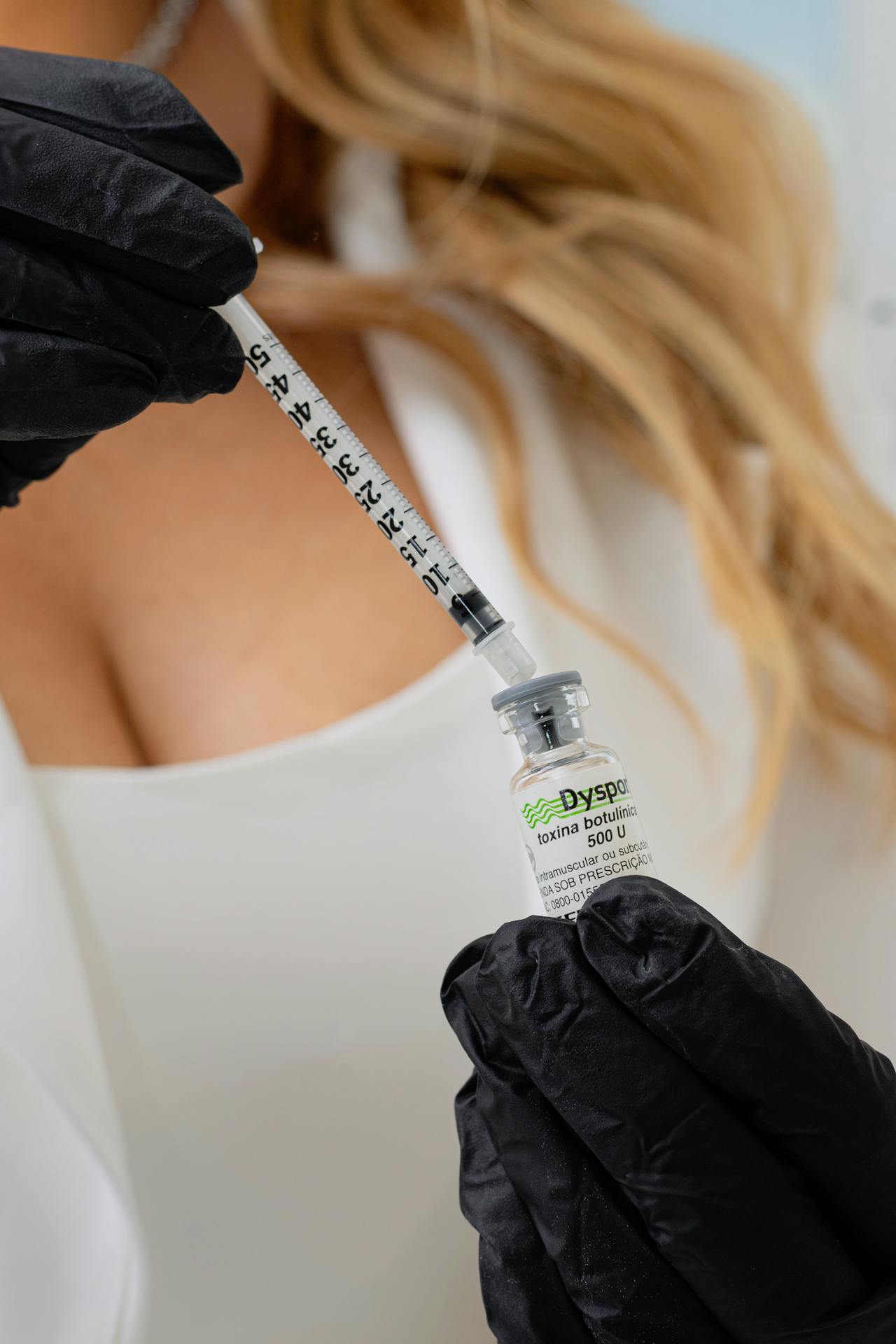
So What About Prevention? Is That Actually a Thing?
Here’s the logic, and it’s surprisingly straightforward.
Expression lines—the ones between your eyebrows, across your forehead, around your eyes—form because you make the same facial movements thousands of times over the years. Every time you squint, frown, or raise your eyebrows, you’re folding the skin in the same spot. When you’re young, the skin bounces back. But over time, collagen breaks down, skin loses elasticity, and those temporary creases start becoming permanent etchings.
Botox temporarily relaxes the muscles that cause these movements. If the muscle isn’t contracting as forcefully, the skin isn’t folding as deeply or as often.
The idea behind preventive Botox is simple: if you reduce the repetitive folding before the lines become etched in, you may be able to delay or minimize the formation of deep static wrinkles—the kind that show up even when your face is completely at rest.
What the Research Shows: Is Botox Really preventive?
A 2022 evidence-based review published in the Journal of Cosmetic Dermatology looked at both clinical studies and real-world practice patterns for Botox in younger adults. The researchers reviewed high-quality randomized controlled trials and surveyed 141 aesthetic practitioners across multiple countries.
Here’s what they found: wrinkle prevention was the number one reason younger patients sought Botox treatment. Not correction—prevention. And the clinical data backed up the approach.
The study’s conclusion was clear: an individualized approach with lower doses for younger adults is recommended, and the clinical evidence supports Botox’s efficacy for both treatment and prevention in this age group. The researchers noted that younger patients who started treatment reported feeling “more attractive” and “more confident” compared to older patients who were trying to correct established lines.
What Dermatologists Actually See
There aren’t many 20-year controlled studies comparing identical twins where one got Botox and one didn’t. (Though actually, there is at least one famous case study of twins, and the difference is pretty striking.) What we do have is decades of clinical observation.
Dermatologists who have been practicing for 20+ years can look at their long-term patients and see patterns. Those who started treatments earlier tend to have less severe static lines later. The muscles themselves can actually weaken somewhat over years of treatment, meaning some patients need less product over time, not more.
Does this mean you have to start Botox at 25 or you’ve missed your window? Absolutely not. People see great results starting treatment at any age. But the mechanism behind prevention makes physiological sense, and the clinical observations support it.
What preventive Botox Won’t Do
Here’s where the skeptics have some valid points, because preventive Botox does get oversold sometimes.
It won’t prevent wrinkles caused by sun damage. Those are about collagen breakdown from UV exposure, and Botox doesn’t address that. (Sunscreen does. Wear it.)
It won’t prevent volume loss—the gradual loss of fat and bone density in the face that happens as we age. Botox doesn’t add volume.
It won’t prevent skin laxity or sagging. That’s about skin structure, gravity, and genetics.
What Botox specifically addresses are dynamic wrinkles—the ones caused by muscle movement—and preventing those from becoming static wrinkles. That’s its thing. It’s one piece of a larger picture, and anyone telling you it’s a complete anti-aging solution isn’t being totally honest.
The Cost Question
Let’s talk about this because it’s usually what people are actually worried about underneath everything else.
Treatments typically run somewhere between $300-500 per session depending on what areas you’re treating, and results last around 3-4 months. That can add up.
Is it “a waste of money”? That really depends on what matters to you. People spend money on gym memberships, hair appointments, skincare routines, and plenty of other things that aren’t strictly necessary but make them feel good. Whether Botox fits into that category is pretty personal.
What’s worth knowing is that preventive doses are often smaller than corrective doses. Someone starting in their late 20s might need way less product than someone trying to soften lines that have been deepening for decades. So sometimes starting earlier actually means spending less per visit.
The Bottom Line
Preventive Botox isn’t a scam or some marketing scheme invented to get younger people into the chair. The mechanism is real and well-understood. Reducing repetitive muscle movements reduces repetitive skin folding, which can slow the formation of permanent creases. Clinical experience over decades backs this up.
It’s also not magic. Sun protection, genetics, overall health, skincare—all of that matters too. Botox is one tool, not the whole toolbox.
If you’ve been on the fence about it, or you’ve had someone in your life giving you a hard time about even considering it, hopefully this gives you something more concrete to work with. The best next step is always a conversation with a board-certified dermatologist who can look at your skin, your goals, and give you actual personalized advice instead of a generic sales pitch or a generic dismissal.
You deserve to make this decision with real information, not just opinions.
Aesthetic Dermatology Associates has offices in Media and Paoli, PA. We’re happy to chat through whether preventive or corrective Botox makes sense for you—no pressure, just answers.
Can I Workout After a Skin Biopsy? Managing Activity While Waiting for Results

Getting a skin biopsy can bring up two main concerns: how to care for the biopsy site and the anxiety that comes with waiting for results. If you’re wondering whether you can continue your normal routine—including exercise—and how to manage the days between your procedure and your phone call from the dermatologist, this guide covers what you need to know.
Returning to Exercise After a Skin Biopsy
Can I workout after a skin biopsy? For most patients, the answer is yes—with some sensible precautions.
Light to moderate exercise is usually fine the same day as your biopsy. Walking, stretching, and everyday activities won’t interfere with healing. However, there are a few things to consider:
For the first 48 hours: Keep the biopsy site dry and protected. This means avoiding swimming pools, hot tubs, and activities that cause heavy sweating. If your biopsy is on your leg or arm, high-impact exercises that strain or stretch the area should be postponed for a few days.
After 48 hours: Once you begin changing the bandage daily, you can gradually return to your normal workout routine. Just make sure to cleanse the site and apply fresh petroleum jelly and a clean bandage after exercising.
Listen to your body: If an activity causes pain, pulling, or bleeding at the biopsy site, scale back. Healing takes priority over maintaining your usual fitness schedule.
If you had a punch biopsy with stitches, ask your dermatologist about specific activity restrictions. Stitches may need extra care, and certain movements could delay healing or affect the final appearance of the scar.
How Long Should You Keep a Skin Biopsy Covered?
The initial bandage should stay in place for at least 48 hours. Keeping the site covered and dry during this period protects the wound and allows the earliest stage of healing to begin undisturbed.
After two days, you’ll start a simple daily routine: gently remove the old bandage, clean the area with mild soap and water, apply a thin layer of petroleum jelly, and cover it with a fresh bandage. Continue this for about one week, or until the site has closed and formed a protective layer.
Moist wound care—keeping the biopsy site slightly moist rather than letting it dry out—promotes faster healing and reduces the chance of noticeable scarring.
Skin Biopsy Healing Stages
Understanding the healing process can help set realistic expectations and reduce worry.
Days 1-2: The site may feel tender and show minor redness or swelling. A small amount of bleeding or oozing is normal. The bandage protects the area while initial clotting and tissue repair begin.
Days 3-7: A scab or thin crust usually forms. The surrounding skin may still appear slightly pink. This is the active healing phase, where new skin cells are regenerating beneath the surface.
Weeks 2-3: The scab naturally falls off on its own. The new skin underneath may look pink or lighter than the surrounding area. Avoid picking at the scab—letting it come off naturally minimizes scarring.
Weeks 4 and beyond: The color gradually evens out. Some biopsies leave a small, flat scar that continues to fade over several months. Protecting the area from sun exposure during this time helps prevent darkening or discoloration.
Why Does It Take So Long for Skin Biopsy Results?
One of the most common frustrations patients express is the waiting period. Results typically take 7 to 10 business days, and for many people, this feels like a long time.
Here’s what happens behind the scenes: After your dermatologist removes the tissue sample, it’s sent to a specialized pathology lab. A dermatopathologist—a physician trained to diagnose skin diseases under a microscope—examines thin slices of the tissue that have been processed and stained. This careful analysis takes time because accuracy is essential.
Some cases require additional steps, such as deeper staining techniques or a second pathologist’s review, which can extend the timeline by a few days. Weekends and holidays also affect turnaround time.
While waiting can be difficult, the thoroughness of this process ensures your dermatologist has the most accurate information to guide your care.
Nervous while waiting for biopsy results?

It’s completely normal to feel anxious while waiting for your results. Many patients describe checking their phone repeatedly, replaying the appointment in their mind, or worrying about what the biopsy might reveal.
A few things to keep in mind during this time:
Most biopsies come back benign. The majority of suspicious moles and lesions turn out to be non-cancerous. Common benign findings include seborrheic keratoses (harmless age-related growths), benign nevi (ordinary moles), and actinic keratoses (precancerous spots that are easily treatable).
Early detection is good news. If the biopsy does identify skin cancer—whether basal cell carcinoma, squamous cell carcinoma, or melanoma—finding it early means treatment is typically straightforward and highly successful.
You’ve already taken the most important step. By getting the biopsy done, you’re being proactive about your health. Waiting for results is part of the process, but you’ve already done the hardest part by seeking evaluation.
Avoid online searching. Every biopsy is unique. Reading about other people’s experiences or trying to self-diagnose based on internet descriptions usually increases anxiety rather than providing clarity.
If the waiting becomes overwhelming, reach out to your dermatologist’s office. A brief conversation with a staff member can often provide reassurance and remind you that help is available if needed.
What Happens Next
Once your results are ready, your dermatologist will contact you using the communication method you selected—phone call, secure message, or follow-up appointment. The reports will explain whether the lesion was benign, precancerous, or malignant, and outline any recommended next steps. For benign results, the biopsy report may only need to be reviewed at your next scheduled routine appointment.
If treatment is needed, options vary depending on the diagnosis. Non-cancerous findings may require no further action. Precancerous lesions might be treated with cryotherapy or topical medication. Skin cancers like basal cell carcinoma and squamous cell carcinoma are often removed with a simple excision. Melanoma may require more extensive evaluation and treatment, but early-stage melanoma has excellent cure rates.
When to Call Your Dermatologist
While complications after a skin biopsy are rare, contact your dermatologist if you notice:
- Bleeding that doesn’t stop after applying firm pressure for 10-15 minutes
- Increasing pain, redness, or swelling around the biopsy site
- Pus, unusual drainage, or a foul odor
- Fever or red streaks extending from the wound
These signs are uncommon, but it’s always better to check in early if something doesn’t seem right.
Moving Forward
A skin biopsy is a brief procedure with a clear purpose: to give your dermatologist the information needed to protect your health. The days that follow—caring for the site, adjusting your routine, and waiting for results—are manageable with the right information and a little patience.
Stay active within your comfort level, follow the aftercare instructions you received, and remember that most people who undergo skin biopsies receive reassuring results. If concerns arise, your dermatology team is available to help.
Other Articles You’d Want To Read
Mole Removal & Treatments: What You Need to Know
What to Do Right After a Skin Cancer Biopsy: First 48 Hours
Mohs Surgery or SRT? What Your Dermatologist Considers When Recommending Skin Cancer Treatment
Plaque Psoriasis: What Those Red Patches Mean (And Why There’s No Reason to Panic)

By Dr. Leib, Board-Certified Dermatologist – Aesthetic Dermatology Associates, serving Paoli & Media, PA
You noticed the first patch a few weeks ago. Maybe on your elbow, or your knee. Pink-red, slightly raised, with silvery-white scales on top. Your family doctor mentioned psoriasis, or maybe a friend recognized it from their own experience.
If you’re reading this because you suspect you have plaque psoriasis, you’re probably feeling anxious, confused, and maybe a little overwhelmed by everything you’re finding online. The good news is this: plaque psoriasis, while chronic, is manageable. Understanding what’s happening to your skin is the first step toward getting the right treatment and feeling more like yourself again.
Let’s start with the medical facts – explained in plain language.
What Is Plaque Psoriasis, Exactly?
Plaque psoriasis is a chronic inflammatory condition of the skin. Translation: it’s a long-term condition where your immune system causes inflammation.
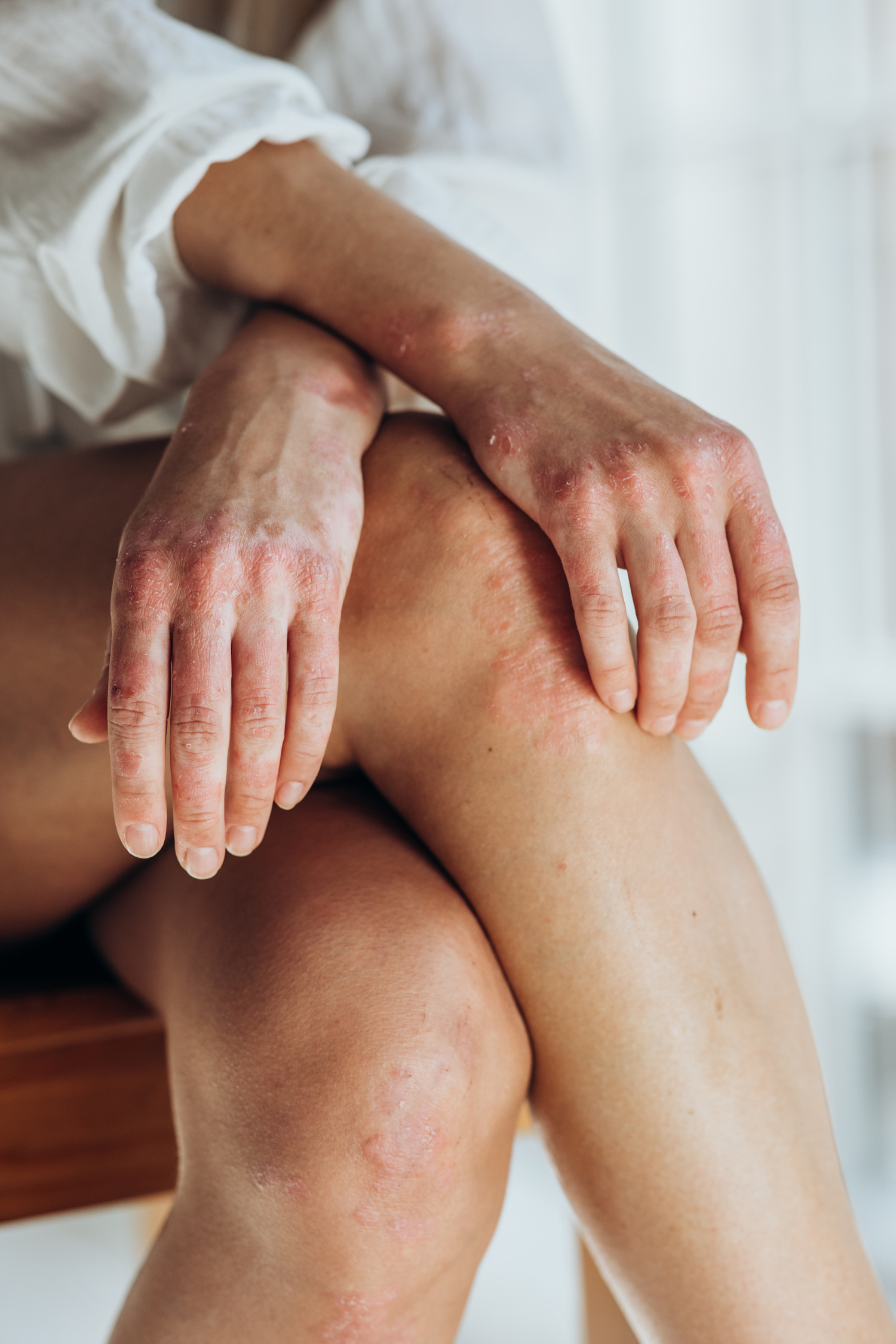
Those raised patches you’re seeing? Dermatologists call them “plaques.” They’re typically pink-red in color with whitish or silvery scales on top. They can appear almost anywhere on your body, but most commonly show up on:
- Knees and elbows (the most common spots)
- Scalp
- Lower back
- Underarms and groin
- Buttocks
- Nails (causing pitting, discoloration, or thickening)
Dr. Leib explains:
“When patients first come in with suspected psoriasis, one of the first things I tell them is: this is not something you caused. It’s not from poor hygiene, something you ate, or anything you did wrong. Plaque psoriasis is an immune-mediated condition – meaning your immune system is the driving force behind what you’re seeing on your skin.”
What Causes Plaque Psoriasis? The Real Answer
This is probably the question weighing most heavily on your mind right now. And here’s the honest answer: like so many medical conditions, the cause of psoriasis is complex. We generally cannot blame one particular thing.
The genetic component:
If you have plaque psoriasis, you have a genetic predisposition. This means you inherited genes that make your immune system more likely to behave this way. You might have family members with psoriasis, or you might be the first person in your family to develop it – both scenarios are common.
Having the genetic tendency doesn’t mean you’ll definitely develop psoriasis. But it does mean that under the right circumstances, your immune system can shift into this overactive state.
Environmental triggers:
Even with genetic susceptibility, something usually acts as a trigger – an environmental factor that essentially “activates” the condition. Common triggers include:
- Stress: Emotional or physical stress is one of the most significant triggers
- Trauma to the skin: Cuts, scrapes, sunburns, or even tattoos can trigger plaques to form at the injury site
- Infections: Strep throat and other infections can trigger psoriasis, especially in younger people
- New medications: Certain drugs, including lithium, beta-blockers, and some blood pressure medications, can trigger or worsen psoriasis
- Weather changes: Cold, dry weather often triggers flares
- Lifestyle factors: Smoking and heavy alcohol use can contribute to development and severity
Dr. Leib emphasizes:
“Many patients come in trying to figure out exactly what caused their psoriasis. While identifying triggers can be helpful for managing the condition, it’s important not to blame yourself. Sometimes we can identify a clear trigger, and sometimes we can’t. Either way, what matters most is moving forward with effective treatment.”
How Common Is Plaque Psoriasis?
You’re far from alone. About 2% of the world’s population is affected by psoriasis, though the frequency is thought to be higher in the United States. That’s millions of people living with this condition.
Psoriasis can occur at any age – from infancy to late adulthood. However, there are two peak times when people are most likely to develop it:
- Ages 20-30 (the most common time for first onset)
- Ages 50-60 (the second peak period)
If you’re being diagnosed in your twenties or thirties, you might feel frustrated that this is happening when you’re supposed to be at your healthiest. But this timing is actually completely typical for plaque psoriasis.
What Does Plaque Psoriasis Feel Like? Recognizing the Symptoms
Unlike eczema (another common inflammatory skin condition), plaque psoriasis tends to be only mildly itchy. Some people experience virtually no itching at all, while others find it bothersome but not severe.
The most common symptoms include:
- Dry, cracked skin
- Stinging or burning sensations, especially if the skin cracks or fissures
- Joint pain or stiffness (if psoriatic arthritis is developing)
A word about cracks and fissures:
Occasionally, psoriasis plaques can cause cracks or fissures in the skin. These can sting, burn, or become painful – especially in areas that bend or flex frequently. These cracks also create an opening for bacteria, which can lead to infections.
If you notice increased warmth, swelling, oozing, or fever alongside your psoriasis, contact your dermatologist right away – these could be signs of infection requiring prompt treatment.
The Psoriatic Arthritis Connection
Here’s something important to know: plaque psoriasis can be associated with psoriatic arthritis – a condition that causes painful inflammation in the joints.
Not everyone with plaque psoriasis will develop psoriatic arthritis, but the two conditions are connected. If you’re experiencing joint pain, stiffness (especially in the morning), or swelling alongside your skin symptoms, mention this to your dermatologist. Catching psoriatic arthritis early and treating it promptly can help prevent permanent joint damage.
Will Plaque Psoriasis Go Away on Its Own?
This is one of the most common questions newly diagnosed patients ask, and it’s important to be honest about the answer.
Even though symptoms aren’t necessarily severe, plaque psoriasis is very stubborn and usually does not go away without treatment. This is one of the key differences between psoriasis and other skin conditions.
Dr. Leib notes:
“I understand that hearing ‘chronic condition’ can feel discouraging. But here’s what that really means: psoriasis is something we manage, not something we cure. And the good news is that we have many, many effective treatment options available today. Although there is no cure for this condition, thankfully there are many treatments that can help minimize the appearance of the plaques and alleviate symptoms. Many of my patients achieve clear or nearly clear skin with the right treatment plan.”
What Happens Next: Your Path Forward
If you’re reading this because you suspect you have plaque psoriasis, the next step is to see a board-certified dermatologist who can:
- Confirm the diagnosis: While plaque psoriasis has characteristic features, other conditions can sometimes look similar. A dermatologist can examine your skin and, if needed, perform a simple biopsy to confirm the diagnosis.
- Assess the severity: Not all psoriasis is the same. Your dermatologist will evaluate how much of your body is affected and how the condition is impacting your quality of life.
- Create a personalized treatment plan: From prescription topical treatments to light therapy to advanced biologic medications, there are numerous options. Your treatment plan will be tailored to your specific situation, preferences, and lifestyle.
- Provide ongoing support: Psoriasis management is a partnership. Your dermatologist will work with you over time to adjust treatments as needed and help you identify and avoid your personal triggers.
You’re Not Alone in This
Finding out you have a chronic skin condition can feel isolating. You might worry about how it looks, whether it will get worse, or how it will affect your daily life.
But here’s what you need to know: plaque psoriasis is highly treatable. With the right dermatology partner and a treatment plan designed for you, most patients see significant improvement. Many achieve clear or nearly clear skin and regain the confidence that psoriasis initially took away.
This condition doesn’t have to define you or limit your life. Treatment works. Relief is possible. And you don’t have to figure this out alone.
About Dr. Leib

Dr. Leib is a board-certified dermatologist with extensive experience treating plaque psoriasis and other complex skin conditions in southeastern Pennsylvania. She served as chief resident during her dermatology training at Virginia Commonwealth University and has contributed to the field through peer-reviewed publications and presentations at regional dermatology conferences.
A Downingtown native and Penn State College of Medicine graduate, Dr. Leib is an active member of leading dermatology specialty societies. She is dedicated to patient-centered care, staying current with the latest treatment advances, and providing compassionate, expert guidance to every patient navigating their psoriasis journey.
Related links:
See Dr. Leib’s provider’s page on our website https://adaderm.com/providers/amy-leib-md/
Review 5-star rating given by patients https://share.google/wJjqWA8m5OvPfw6Hx
Schedule Your Plaque Psoriasis Consultation in Paoli or Media, PA
Understanding what’s happening to your skin is the first step. Getting expert care is the next.
At Aesthetic Dermatology Associates, Dr. Leib and our experienced team offer:
- Accurate diagnosis: Comprehensive evaluation to confirm plaque psoriasis and rule out other conditions
- Personalized treatment plans: Tailored to your lifestyle, severity, and treatment goals
- Full range of treatment options: From prescription topicals to advanced biologic therapies
- Compassionate, expert care: A dermatology partner who understands your concerns and guides you every step of the way
Conveniently serving patients in Paoli, PA and Media, PA
Don’t let uncertainty keep you from getting the care you need. Whether you’re newly diagnosed or seeking better management, we’re here to help you achieve clear, comfortable skin – and peace of mind.
Rosacea on Your Face: What That Redness Means (And Why There’s No Reason to Panic)

By Nancy Conley, PA-C, Diplomate of the Society of Dermatology Physician Assistants – Aesthetic Dermatology Associates, serving Paoli & Media, PA
Your face has been turning red more than usual. At first, you thought it was just from the heat, or maybe that glass of wine at dinner. But now the redness lingers. Your cheeks seem perpetually flushed, and you’ve noticed small bumps that almost look like acne – except your go-to acne cream isn’t helping at all.
Maybe your doctor mentioned the word “rosacea” during your last visit. Or perhaps a friend who has it recognized the telltale signs. Now you’re online at night, scrolling through images and articles, asking yourself:
Is this really what’s happening to my face? What caused this? And can I make it go away?
If you’re here because you think you might have rosacea, you’re likely feeling self-conscious, frustrated, and worried about what this means for your skin going forward. Here’s what you need to hear right now: rosacea is one of the most common facial skin conditions, and it responds incredibly well to proper treatment. You’re not stuck with persistent redness and sensitivity. Understanding what’s causing your symptoms is the first step toward skin that looks and feels healthy again.
Let’s talk about what’s really happening – in terms that actually make sense.
The Truth About Rosacea: It’s More Than Just Blushing

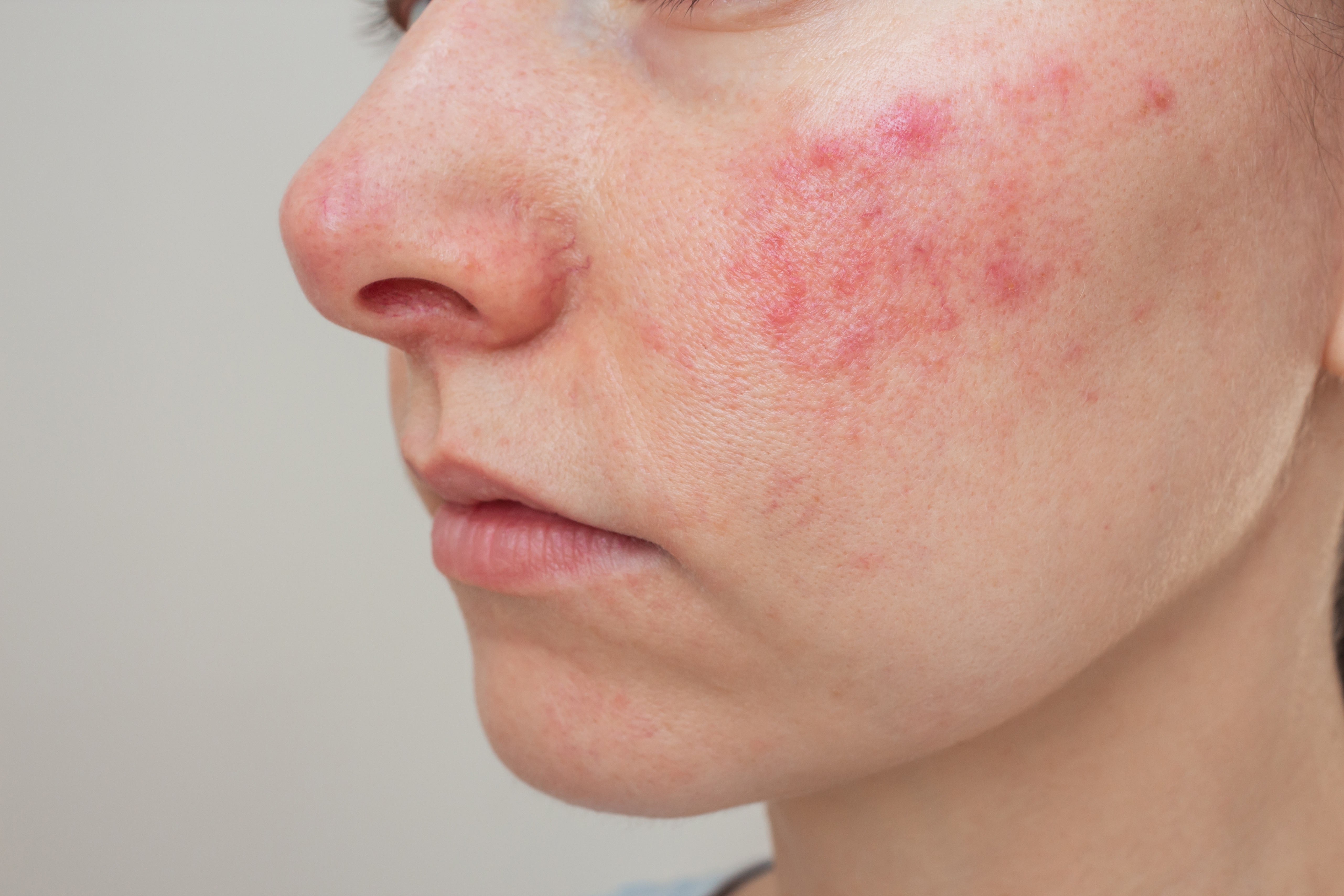
Rosacea is a chronic inflammatory skin condition that primarily affects the face. In practical terms, this means your facial blood vessels and oil glands react more intensely than they should to certain triggers, causing visible redness, flushing, and sometimes acne-like breakouts.
Here’s what makes rosacea different from just having “sensitive skin” or occasional flushing:
The symptoms persist. That rosy glow or facial redness doesn’t fully fade the way a normal flush would. For many people, there’s a baseline redness that’s always there, punctuated by episodes where it gets much worse.
The symptoms come and go in waves. You might have weeks where your skin looks relatively calm, followed by a flare-up where everything gets worse – more redness, more bumps, more discomfort. These flare-ups are usually triggered by specific factors (more on that in a moment).
You might be experiencing:
- Redness that won’t fade, especially across your nose, cheeks, chin, and forehead
- A face that flushes easily and intensely
- Tiny red or purple blood vessels visible just under your skin
- Bumps and small pimples that appear without warning
- Skin that stings, burns, or feels uncomfortably tight
- Rough, dry patches even when you’re moisturizing
- A sensation of heat in your face
- Eyes that feel irritated, dry, or bloodshot
Nancy Conley explains:
I see patients every day who are self-conscious about their red, acne prone skin. When I tell them it’s rosacea and I can treat it, there is a moment of relief. Then we jump into the nitty gritty – what it is and how I can help.
The Trigger Puzzle: Why Your Face Flares Up
Even though we can’t always prevent rosacea from developing, we can absolutely identify and manage the things that make it worse. These are called triggers, and they’re different for everyone.
The most common culprits include:
Sun exposure: This is the number one trigger for most people with rosacea. UV rays cause blood vessels to dilate and inflammation to increase. Even brief sun exposure can cause a flare that lasts for days.
Alcohol consumption: Wine (especially red wine), beer, and spirits all commonly trigger facial flushing and redness in people with rosacea.
Spicy foods: Anything with heat – hot peppers, curry, hot sauce – can cause your face to flush and stay red for hours.
Temperature extremes: Very hot or very cold environments, or moving quickly between them (like going from air conditioning into summer heat), can trigger symptoms.
Hot beverages: That morning coffee or afternoon tea might be contributing to your facial redness, especially if you drink it while it’s very hot.
Stress and strong emotions: Emotional stress, anxiety, anger, or embarrassment can all cause flushing and worsen rosacea.
Harsh skincare products: Products with fragrances, alcohol, exfoliating acids, or rough physical scrubs can irritate rosacea-prone skin and trigger flares.
Intense exercise: While exercise is healthy, the flushing and heat it generates can worsen rosacea for some people.
Living With Rosacea: What It Actually Feels Like Day-to-Day
Beyond the visible redness and bumps, rosacea affects how your skin feels and how you feel about your skin.
Physically, many people describe:
- A burning or stinging sensation, especially when applying products
- Tightness, like your skin is too small for your face
- Constant awareness of warmth in your cheeks or nose
- Discomfort that gets worse throughout the day
- Sensitivity to products you used to tolerate just fine
Emotionally, rosacea can take a toll:
- Self-consciousness about your appearance
- Frustration when flare-ups happen unpredictably
- Anxiety about social situations where you might flush
- Feeling like you have to explain your “red face” to people
- Avoiding activities (like hot yoga or spicy dinners) that you used to enjoy
These feelings are completely valid. Your skin is on your face – the most visible part of your body. Of course it affects how you feel. This is exactly why getting proper treatment isn’t vanity; it’s taking care of your well-being.
The Bottom Line: Will It Get Better Without Treatment?
Here’s what you need to know: rosacea rarely improves on its own. In most cases, without treatment, it actually gets progressively worse over time.
What might start as occasional flushing can evolve into permanent redness. Small bumps can become more frequent and widespread. In some cases, the skin can thicken, particularly around the nose.
Nancy Conley is direct about this:
I never want to scare patients, but I want to them to understand control is attainable. While there is no cure for this condition, thankfully many treatments are available to give you your best skin. Whether you’ve only had symptoms for a few months, or even symptoms for many years, we can achieve significant improvement and prevent progression!
Building Your Rosacea-Friendly Skincare Routine
Before prescription treatments, let’s talk about the foundation: how you care for your skin every single day. For rosacea, gentle skincare isn’t optional – it’s essential.
The golden rule: sensitive skin care is key.
Your skin barrier is compromised when you have rosacea. It’s more reactive, more sensitive, and less able to tolerate products and ingredients that other people use without issue. This means you need to completely rethink your skincare approach.
Products to avoid completely:
- Anything fragranced, even if it says “natural fragrance”
- Exfoliants of any kind – no scrubs, no acids, no chemical peels
- Alcohol-based toners or astringents
- Witch hazel
- Menthol, peppermint, eucalyptus, or other “cooling” or “tingling” ingredients
- Rough washcloths, loofahs, or cleansing brushes
- Hot water on your face
What your face wash should be:
Choose a gentle facial cleanser specifically formulated for sensitive skin. Look for something creamy, non-foaming, and fragrance-free. Alternatively, Nancy Conley recommends a medicated sulfur cleanser, which can help calm inflammation while still cleansing effectively.
Wash with lukewarm (not hot) water, using only your fingertips. Pat dry gently with a soft towel – don’t rub.
When your skin is flaring:
A hydrating face mask can provide immediate relief during a flare-up. Nancy specifically recommends Skinceuticals Phyto Corrective Mask for its ability to instantly calm irritated, inflamed skin. Keep it in your skincare arsenal for those days when your face feels particularly angry.
Sun protection – non-negotiable:
Every single day, rain or shine, winter or summer, you need sunscreen. Choose a mineral-based formula (zinc oxide or titanium dioxide) with at least SPF 30. Chemical sunscreens can sometimes irritate rosacea-prone skin, so mineral formulas are generally safer.
Moisturizer matters:
Even if your skin feels oily or you have acne-like bumps, you need a good moisturizer. Choose something designed for sensitive skin, fragrance-free, and with soothing ingredients like ceramides or niacinamide.
Medical Treatments That Make a Real Difference
The right skincare routine sets the foundation, but for most people with rosacea, medical treatment is what really transforms the skin.
Topical prescription creams:
Multiple prescription medications can reduce redness, calm inflammation, and minimize bumps and visible blood vessels. These are typically applied once or twice daily and work by targeting the specific inflammatory processes happening in rosacea-affected skin.
Oral antibiotics:
For moderate to severe rosacea, especially when you have significant bumps and pustules, oral antibiotics can provide dramatic improvement. These work by reducing inflammation throughout your body, not by fighting infection. They’re typically used for a limited time to get symptoms under control.
Laser and light treatments:
Advanced laser therapies can specifically target the visible blood vessels and persistent background redness that topical treatments sometimes can’t fully address. These treatments provide long-lasting improvement and can significantly reduce the overall redness of your complexion.
Why one-size-fits-all doesn’t work:
Your rosacea is unique to you. The severity, the specific symptoms, your skin type, your lifestyle, your budget, your treatment preferences – all of these factors matter when creating a treatment plan.
Nancy Conley explains her approach:
When I sit down with a rosacea patient, I want to understand the whole picture. What bothers you most – the redness, the bumps, the sensitivity? What have you already tried? What’s your daily routine like? Are you willing to take an oral medication, or would you prefer to stick with topical treatments? Do you want to consider laser therapy? It’s always best to consult with your dermatology provider to discuss treatment options that would be best for your particular skin. This is a collaborative process, and my job is to help you find the approach that works for your life and your goals.
Taking the Next Step: Getting Professional Help
If you’ve read this far and you’re recognizing yourself in these descriptions, it’s time to see a dermatology provider who can give you a definitive diagnosis and start you on the path to clearer skin.
Here’s what to expect when you come in for a consultation:
Comprehensive skin evaluation: Your provider will examine your face closely, ask about your symptoms and their timeline, and discuss your skincare routine and lifestyle factors. In most cases, rosacea can be diagnosed based on appearance and history alone, without any testing needed.
Customized treatment strategy: Based on your specific symptoms, skin type, and preferences, your provider will recommend a treatment plan. This might include skincare changes, prescription medications, laser treatments, or a combination of approaches.
Ongoing partnership: Rosacea is a chronic condition, which means your treatment might need adjustments over time. Your dermatology provider will follow your progress, modify your treatment as needed, and help you navigate challenges as they come up.
You don’t have to live with constant redness and sensitivity. You don’t have to avoid activities you love or feel self-conscious about your appearance. Treatment works. Relief is real. And you absolutely don’t have to figure this out alone.

About Nancy Conley, PA-C
Nancy Conley, is a board-certified Physician Assistant specializing in medical and cosmetic dermatology, with particular expertise in treating rosacea and sensitive skin conditions. As a Diplomate of the Society of Dermatology Physician Assistants (SDPA) – a distinction earned by only a select group of PAs nationwide – Nancy has completed advanced dermatology-specific training that enables her to provide expert care for even the most challenging rosacea cases.
A Philadelphia-area native and proud member of the Aesthetic Dermatology Associates team, Nancy is known for her patient-centered approach to rosacea treatment. She takes time to understand each patient’s unique triggers, lifestyle factors, and treatment goals, creating customized care plans that deliver real results. Licensed in Pennsylvania, Nancy combines clinical excellence with genuine compassion, helping patients achieve clear, calm, confident skin.
Related link:
See Nancy’s provider’s page on our website.
Get Expert Rosacea Care in Paoli or Media, PA
Understanding what’s happening to your face is empowering. Getting the right treatment is life-changing.
At Aesthetic Dermatology Associates, Nancy Conley and our experienced team provide:
- Accurate rosacea diagnosis: Thorough evaluation to confirm rosacea and identify your specific subtype
- Customized treatment plans: Designed around your unique skin, lifestyle, and goals
- Complete range of solutions: From gentle skincare guidance to prescription medications to advanced laser therapies
- Expert, compassionate care: A partner who listens to your concerns and supports you through every step of your treatment journey
Conveniently located to serve patients throughout Paoli, PA and Media, PA
Don’t let facial redness and sensitivity hold you back from feeling confident in your skin. Whether you’re just noticing symptoms or you’ve been struggling with rosacea for years, we’re here to help you achieve the clear, calm, comfortable skin you deserve.
Plaque Psoriasis Treatment Options: From Topicals to Biologics

By Dr. Patel, Board-Certified Dermatologist – Aesthetic Dermatology Associates, serving Paoli & Media, PA.
Here’s the truth: currently there is no complete cure for psoriasis. However, there are numerous treatment options available, and they are often quite effective.
At Aesthetic Dermatology Associates, treatment is tailored to each patient’s specific situation. Here are the options that may be recommended:
1. Topical Therapies
These include agents that decrease inflammation and reduce flaking of the skin. Topical treatments are often the first line of defense, especially for mild to moderate psoriasis.
Common topical medications include:
- Corticosteroids (various strengths depending on location and severity)
- Vitamin D analogues (calcipotriene)
- Retinoids (tazarotene)
- Calcineurin inhibitors (tacrolimus, pimecrolimus)—especially useful for sensitive areas like the face
- Topical Small Molecule inhibitors
- Coal tar preparations
- Salicylic acid—helps remove scales
2. Injection of Steroid Medication
Dr. Patel explains:
“For stubborn plaques that aren’t responding to topical treatments, we can inject steroid medication right into the affected areas of skin. This delivers the anti-inflammatory effect of the steroid directly where it’s needed most. These injections cause minimal and temporary discomfort and are very quick.”
These intralesional injections are quick, performed in the office, and can be particularly effective for thick plaques on elbows, knees, or scalp.
3. Ultraviolet Light Therapy
Ultraviolet light has anti-inflammatory effects on the skin and can be highly effective for widespread or localized psoriasis.
Dr. Patel states:
“Photherapy is a really safe and effective way to treat psoriasis. It has a long history of effective use in dermatology for a variety of skin conditions. However, it requires consistency over a long period of time. At ADA we have full body treatment units along with localized phototherapy lasers for stubborn areas.”
Light therapy typically requires coming to the office 2-3 times per week initially, then tapering to maintenance sessions.
4. Oral Medications
For moderate to severe psoriasis, systemic medications, including oral medications, may be appropriate.
These may include:
- Traditional agents like methotrexate, which has been used for decades and works by suppressing the overactive immune response
- Newer agents like Otezla (apremilast), which works by inhibiting an enzyme involved in inflammation
These medications work through a variety of mechanisms to calm the immune system’s overactivity.
5. Biologic Medications
Dr. Patel notes:
“You’ve probably seen several ads online and on TV for many of these medications!”
These injectable medications represent some of the most significant advances in psoriasis treatment. Biologics work by blocking specific inflammatory chemicals in the body—targeting the exact immune pathways involved in psoriasis. They include drugs like:
- TNF-alpha inhibitors (Humira, Enbrel, Remicade)
- IL-17 inhibitors (Cosentyx, Taltz, Siliq, Bimzelx)
- IL-23 inhibitors (Skyrizi, Tremfya, Ilumya)
- IL-12/23 inhibitor (Stelara)
*all brands above copyrighted
These medications have transformed treatment for many patients with moderate to severe psoriasis, often achieving near-complete skin clearance.
Dr. Patel emphasizes:
“All medications have potential benefits, side effects, treatment schedules and risks. These will be reviewed with you by your provider so you can make an informed decision.”
I Feel Overwhelmed With All These Options—How Can I Make a Decision?

This is a common and completely understandable reaction. The good news is: you’re not making this decision alone.
Dr. Patel reassures patients:
“Our job at ADA is to work with you to come up with a plan that maximizes effectiveness while attempting to minimize risk. We’ll find the right approach for you!”
Some factors that may go into the decision of which therapy to try include:
- Your desire or willingness to apply topical medications on a regular basis
- Your schedule availability for light therapy (which requires multiple office visits per week)
- Your risk tolerance for side effects
- Your willingness to have small injections
- The severity and location of your psoriasis
- Other medical conditions you may have
- Medications you’re currently taking
- Your lifestyle and treatment preferences
- Cost and insurance coverage
Dr. Patel adds:
“Often topical therapies will be tried before anything else. However, for severe disease, a systemic medication or light therapy may be recommended right away.”
The approach taken depends entirely on your individual situation. There’s no one-size-fits-all answer—and that’s actually a good thing. It means treatment can be customized to fit your life, not force your life to fit around treatment.
What Your Dermatologist Wants You to Know About Living With Psoriasis
After treating hundreds of patients with psoriasis throughout his career—from his training at the University of Texas Southwestern to his work in the Philadelphia area—Dr. Patel has learned that successful psoriasis management is about partnership.
Here’s what every patient should understand:
Long-term management is absolutely possible. While there’s no cure, most patients will see significant improvement in their psoriasis by following a customized treatment protocol tailored for their specific needs. Many patients achieve months or even years of clear or nearly clear skin.
You’re not failing if you flare. Psoriasis is unpredictable. Even with perfect adherence to treatment, flares can happen. That doesn’t mean the treatment isn’t working or that you’ve done something wrong—it means the treatment plan may need adjustment.
Your mental health matters just as much as your skin. The psychological burden of psoriasis is real. The itching, the visible plaques, the impact on your social life and self-esteem—all of this affects your quality of life. If you’re struggling emotionally, tell your dermatologist. There are resources available, and addressing the emotional aspect is part of treating the whole person, not just the skin condition.
Consistency is key. One of the biggest challenges is when patients stop their treatment as soon as their skin clears. Psoriasis is a chronic condition. Maintaining your treatment—even when you’re doing well—helps prevent the next flare.
Dr. Patel emphasizes:
“Fortunately, as a patient of Aesthetic Dermatology Associates, we will be with you while making the decision of which therapies to try, and as you proceed with treatment. We will see you on a regular basis and we are always a phone call or a text away. If you change your mind about a particular therapy, we’ll work with you to find an acceptable alternative.”
You Don’t Have to Navigate This Alone
If you’re experiencing a psoriasis flare-up right now, the urgency you feel is completely understandable. You want relief, you want answers, and you want to know that someone understands what you’re going through.
That’s exactly what dermatologists are here for.
Psoriasis treatment has come incredibly far in recent years. The options available today—from advanced biologics to targeted light therapy—offer hope that wasn’t available even a decade ago. But the key is finding the right treatment combination for you, and then adjusting it as needed over time.
Dr. Patel concludes:
“Most patients will see significant improvement in their psoriasis by following a customized treatment protocol tailored for their specific needs.”
From first-time flare-ups to long-term management, expert dermatological care makes all the difference. Collaborating with the right team allows you to build a personalized treatment strategy that aligns with your daily routine, tackles your specific challenges, and delivers the clear, comfortable skin you’ve been seeking. Managing this condition shouldn’t mean sacrificing the life you want to live.
Arrange a Psoriasis Treatment Consultation in Paoli or Media, PA
Living with psoriasis means having a dermatology partner who understands your unique challenges and stays with you through every treatment decision. At Aesthetic Dermatology Associates, Dr. Altman and our experienced team offer:
- Comprehensive treatment options: From prescription topicals to cutting-edge biologics
- Same-week appointments: Priority scheduling available for severe flare-ups
- Personalized care plans: Tailored to your lifestyle, preferences, and treatment goals
- Ongoing support: Direct access to your care team when you need guidance
Conveniently serving patients in Paoli, PA and Media, PA
Don’t wait for your next flare-up to take action. Whether you’re newly diagnosed or seeking better management of long-standing psoriasis, we’re here to help.
About the Author

Dr. Patel is a board-certified dermatologist with advanced training in medical, surgical, and cosmetic dermatology. An Adjunct Associate Professor at the University of Pennsylvania Perelman School of Medicine in Philadelphia, he has authored peer-reviewed research and mentored future dermatologists.
At Aesthetic Dermatology Associates, Dr. Patel specializes in skin cancer diagnosis and treatment, medical dermatology, and patient education. He proudly serves the communities of Paoli, Media, and the greater Philadelphia Main Line area, providing compassionate, evidence-based dermatologic care.
Related links
See Dr. Patel’s personal page on our website
Follow Dr. Patel on LinkedIn professional social network
Review Dr. Patel’s rating on US News Health website
Psoriasis Flare-Up: What’s Happening to Your Skin and How to Regain Control

By Jamie Altman, MD, Board-Certified Dermatologist – Aesthetic Dermatology Associates, serving Paoli & Media, PA
Waking up to see new patches spreading across your skin can be frightening. The itching keeps you up at night. Plans get canceled because of worry about people staring. And the question that haunts most:
Is this ever going to stop?
If you’re reading this during a psoriasis flare-up, you’re probably feeling a mix of panic, frustration, and exhaustion. Maybe you’ve been managing psoriasis for years, or maybe this is your first severe episode. Either way, what you’re experiencing is your immune system overreacting—not your body “getting worse forever.” And more importantly, there are clear steps that can be taken to help you regain control.
You’re Not Imagining It—Here’s What’s Happening Right Now
During a psoriasis flare-up, the immune system has shifted into overdrive. Normally, skin cells take about 28-30 days to grow and shed. But in psoriasis, this process speeds up to just 3-4 days. Your body is producing skin cells faster than it can shed them, causing those thick, scaly patches—what dermatologists call plaques.
Dr. Altman explains:
“This isn’t about poor hygiene or something you did wrong. Psoriasis is an immune-mediated condition. Your immune system is mistakenly stimulating healthy skin cells, causing rapid cell turnover.”
Does Psoriasis Spread?
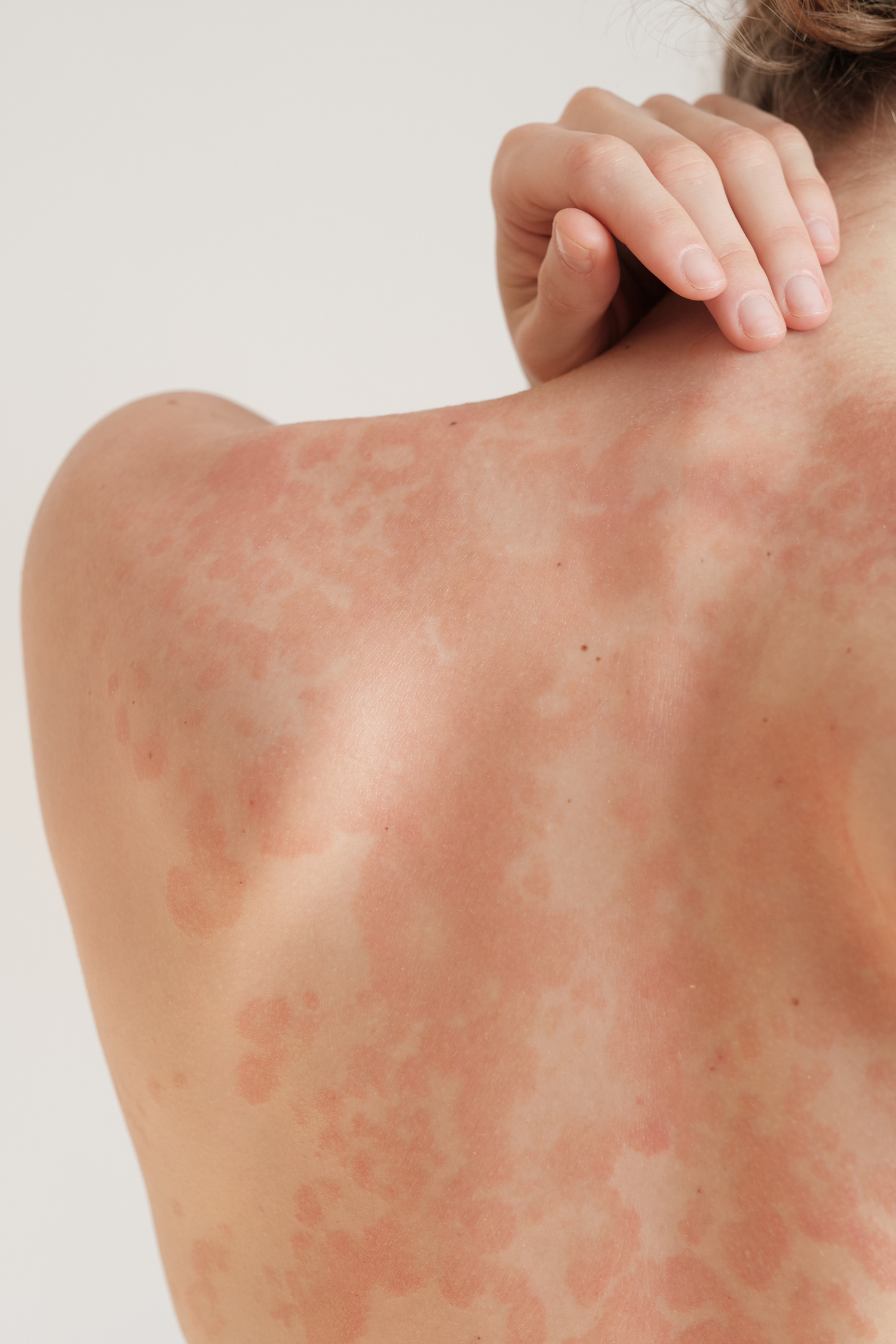
This is one of the most common questions during flare-ups, and it’s important to address directly: psoriasis is not contagious. You cannot spread it to others, and others cannot catch it from you.
However, existing patches can expand, and new patches can appear in different areas of your body—especially during a flare-up. This isn’t the condition “spreading” like an infection; it’s your immune system triggering inflammation in multiple areas. Psoriasis can also appear at sites of skin injury—a phenomenon called the Koebner response. A cut, scrape, sunburn, or even a tattoo can trigger new patches to form.
Dr. Altman notes:
“When patients see new patches appearing, they understandably panic. But this is your immune system’s response pattern, not a sign that something catastrophic is happening. With proper treatment, we can calm this immune response and help your skin heal.”
What Triggered This? Common Culprits Behind Psoriasis Flare-Ups
Understanding what causes psoriasis flare-ups can help you identify patterns—though it’s important to note: sometimes there’s no obvious trigger, and that’s not your fault.
Common triggers include:
- Stress: Emotional or physical stress is one of the most significant triggers. Your body releases inflammatory chemicals when you’re stressed, which can activate psoriasis.
- Infections: Strep throat, respiratory infections, or even a simple cold can trigger flares, especially in people with guttate psoriasis.’
- Medications: Some drugs, including lithium, beta-blockers, antimalarial drugs, and NSAIDs, can worsen psoriasis.
- Weather changes: Cold, dry weather often triggers flares because low humidity dries out the skin.
- Skin injury: Cuts, scrapes, bug bites, severe sunburn—any trauma to the skin can trigger new patches.
- Alcohol and smoking: Both can worsen psoriasis and reduce the effectiveness of treatments.
Sometimes, despite your best efforts to avoid triggers, flares still happen. This doesn’t mean you’re doing something wrong. Psoriasis has its own rhythm, and sometimes the immune system responds to factors we can’t fully identify or control.
Extreme Psoriasis vs. Regular Flare: When to Call Your Dermatologist Immediately

Not all flares are the same. While most can be managed with adjustments to your treatment plan, some situations require immediate medical attention.
Call your dermatologist right away if you experience:
- Sudden, widespread coverage: If psoriasis is rapidly covering large areas of your body (more than 10% of your skin surface).
- Pustular psoriasis: If you develop pus-filled blisters along with fever, chills, or feeling generally unwell. This is a medical emergency.
- Erythrodermic psoriasis: If most of your body becomes red, inflamed, and you’re experiencing severe pain or temperature regulation problems. This is also a medical emergency.
- Severe joint pain or swelling: This could indicate psoriatic arthritis, which requires prompt treatment to prevent joint damage.
- Signs of infection: Increased warmth, swelling, oozing, or fever alongside your psoriasis patches.
Dr. Altman emphasizes:
“I never want patients to worry about ‘bothering’ me during a severe flare. Extreme psoriasis requires immediate intervention. That’s what we’re here for. If you’re unsure whether your flare warrants a call, err on the side of caution and reach out.”
Your Action Plan: What You Can Do in the Next 24 Hours
When you’re in the middle of a flare, you need relief now. Here’s what you can start doing today while you connect with your dermatologist:
Immediate relief strategies:
- Moisturize aggressively: Apply thick, fragrance-free moisturizers or ointments (like petroleum jelly or Aquaphor) multiple times per day, especially right after bathing when your skin is still damp. This helps seal in moisture and reduce scaling.
- Take lukewarm baths: Add colloidal oatmeal, Dead Sea salts, or bath oil. Soak for 10-15 minutes to soften scales. Avoid hot water—it strips your skin’s natural oils and worsens inflammation.
- Use over-the-counter hydrocortisone: For light psoriasis or small areas, OTC 1% hydrocortisone cream can provide temporary relief. Apply as directed on the package.
- Apply cool compresses: If itching or burning is severe, cool (not ice-cold) compresses can help calm the inflammation.
- Avoid your known triggers: If you know certain foods, alcohol, or stress worsen your flares, now is the time to be especially vigilant.
- Protect your skin: Avoid scratching (which can create new patches through the Koebner response), wear soft cotton clothing, and be gentle when drying off after bathing—pat, don’t rub.
These measures can help you feel more comfortable while you work with your dermatologist on a comprehensive treatment plan. But they’re not substitutes for medical treatment, especially during severe flares.
How to Prevent the Next Flare-Up (Or Make It Less Severe)
While we can’t prevent every flare-up, there are strategies that can reduce their frequency and severity:
Daily skin care routine: Consistent moisturizing is your foundation. Even when your skin looks clear, maintaining your skin barrier helps prevent future flares.
Stress management: Since stress is a major trigger, finding effective stress-reduction techniques—whether that’s exercise, meditation, therapy, or simply better sleep—can make a significant difference.
Stick with your treatment plan: One of the most common reasons for flares is stopping treatment too soon when skin clears. Psoriasis is chronic; maintaining treatment helps keep it in remission.
Track your triggers: Keep a journal of flares and potential triggers. Over time, you may identify patterns that help you avoid certain situations or products.
Maintain a healthy weight: There’s a connection between obesity and psoriasis severity. Weight loss can improve treatment response.
Limit alcohol: Alcohol can trigger flares and interfere with medication effectiveness.
Dr. Altman advises: “I tell my patients: you can’t control everything about psoriasis, but you can control your response to it. Building a consistent skin care routine and working with your dermatology team to adjust treatments as needed puts you back in the driver’s seat.”
Whether you’re dealing with your first flare or you’ve been managing psoriasis for years, expert help is available to help you regain control. Working together with a dermatology team, you can create a treatment plan that fits your life, addresses your concerns, and gives you the clear, comfortable skin you deserve.
Because living with psoriasis shouldn’t mean putting your life on hold.
About Dr. Jamie Altman
Dr. Altman is a board-certified dermatologist and Chief of the Subdivision of Dermatology at Riddle Memorial Hospital. He completed his dermatology residency at the University of Michigan and advanced fellowship training in skin cancer treatment at Memorial Sloan-Kettering Cancer Center in New York City. A former Clinical Instructor in Dermatology at the University of Pennsylvania, Dr. Altman has been recognized as a Top Dermatologist by U.S. News & World Report and a Top Doctor by Philadelphia Magazine (2013–2020). He served as President of the Philadelphia Dermatological Society (2020–2021) and is committed to providing compassionate, expert care to every patient.
Related links
See Dr. Altman’s provider’s page on our website
Follow Dr. Patel on LinkedIn professional social network
Review Dr. Patel’s rating on US News Health website
Arrange a Psoriasis Treatment Consultation in Paoli or Media, PA
Living with psoriasis means having a dermatology partner who understands your unique challenges and stays with you through every treatment decision. At Aesthetic Dermatology Associates, Dr. Altman and our experienced team offer:
- Comprehensive treatment options: From prescription topicals to cutting-edge biologics
- Same-week appointments: Priority scheduling available for severe flare-ups
- Personalized care plans: Tailored to your lifestyle, preferences, and treatment goals
- Ongoing support: Direct access to your care team when you need guidance
Conveniently serving patients in Paoli, PA and Media, PA
Don’t wait for your next flare-up to take action. Whether you’re newly diagnosed or seeking better management of long-standing psoriasis, we’re here to help.
Mohs Surgery or SRT? What Your Dermatologist Considers When Recommending Skin Cancer Treatment

By Dr. Patel, Board-Certified Dermatologist – Aesthetic Dermatology Associates, serving Paoli & Media, PA
When you’re diagnosed with skin cancer, one of the first questions that comes to mind is:
“What’s the best treatment for me?”
It’s completely normal to feel uncertain — especially if your dermatologist recommends multiple treatment options, like Mohs surgery or Superficial Radiation Therapy (SRT).
At Aesthetic Dermatology Associates, we understand that choosing the right approach can feel overwhelming. The truth is, your doctor’s recommendation isn’t random. It’s based on specific medical, anatomical, and personal factors designed to give you the best long-term outcome with the least disruption to your life.
Let’s walk through what we, as dermatologists, consider when recommending Mohs surgery versus radiation treatment for skin cancer — so you can feel informed, reassured, and confident in your care plan.
Understanding the Types of Skin Cancer
There are three major forms of skin cancer that dermatologists treat most frequently:
- Basal cell carcinoma (BCC): The most common type, usually slow-growing and highly treatable. It rarely spreads beyond the original site and responds exceptionally well to treatments such as Mohs surgery or Superficial Radiation Therapy (SRT).
- Squamous cell carcinoma (SCC): Can grow more quickly and occasionally spread if not treated early, but when caught in its early stages, it also carries an excellent prognosis. Treatments are highly effective, and recurrence rates are very low with proper follow-up.
- Melanoma: The least common but most serious of the three most well known forms of skin cancer, arising from pigment-producing cells called melanocytes. While melanoma requires prompt surgical removal, early detection dramatically improves outcomes — with five-year survival rates above 99% when caught at an early stage. Modern advances in targeted therapy and immunotherapy have also made later-stage melanomas far more manageable than in the past.
The good news is that nearly all skin cancers — including melanoma when detected early — are highly curable. Regular skin checks, quick evaluation of new or changing moles, and timely treatment make a life-changing difference.
Dr. Patel reminds patients:
“Hearing the word skin cancer can sound frightening, but today’s treatments are incredibly effective. With early diagnosis, we can almost always achieve excellent results and peace of mind.”
Mohs Surgery: The Gold Standard for Precision
Mohs micrographic surgery is often called the gold standard for treating many basal and squamous cell skin cancers — especially those in delicate or cosmetically sensitive areas such as the face, ears, nose, eyelids, scalp, hands, and genitals.
How Mohs Surgery Works
The area is numbed with local anesthesia.
The dermatologist surgically removes a thin layer around the cancerous tissue.
While you wait comfortably in the office, the tissue is examined under a microscope to check the margins — with the goal of ensuring every cancer cell has been removed.
If cancer cells are still present, another layer is removed and tested, repeating the process until the margins are clear.
Once the area is cancer-free, the wound is closed, often with fine sutures.
This method allows the surgeon to preserve as much healthy tissue as possible while achieving the highest possible cure rate — typically up to 99% for many non-melanoma skin cancers.
What to Expect After Mohs Surgery
Some visible scarring is expected, though careful suturing and good wound care minimize it.
Bruising, swelling, and mild pain may occur for a few days.
Infection risk is low but possible.
Recovery depends on wound size and location — often 1–3 weeks for full healing.
Dr. Patel emphasizes:
“Mohs surgery provides unmatched accuracy. We’re able to see exactly where the cancer ends and stop there — which is especially important for preserving appearance and function in areas like the nose, eyelids, and lips.”
Superficial Radiation Therapy (SRT): A Non-Surgical Alternative
For some patients, Superficial Radiation Therapy (SRT) offers a non-invasive, highly effective way to treat certain types of basal and squamous cell skin cancers — particularly on the head, neck, and other difficult-to-treat areas.
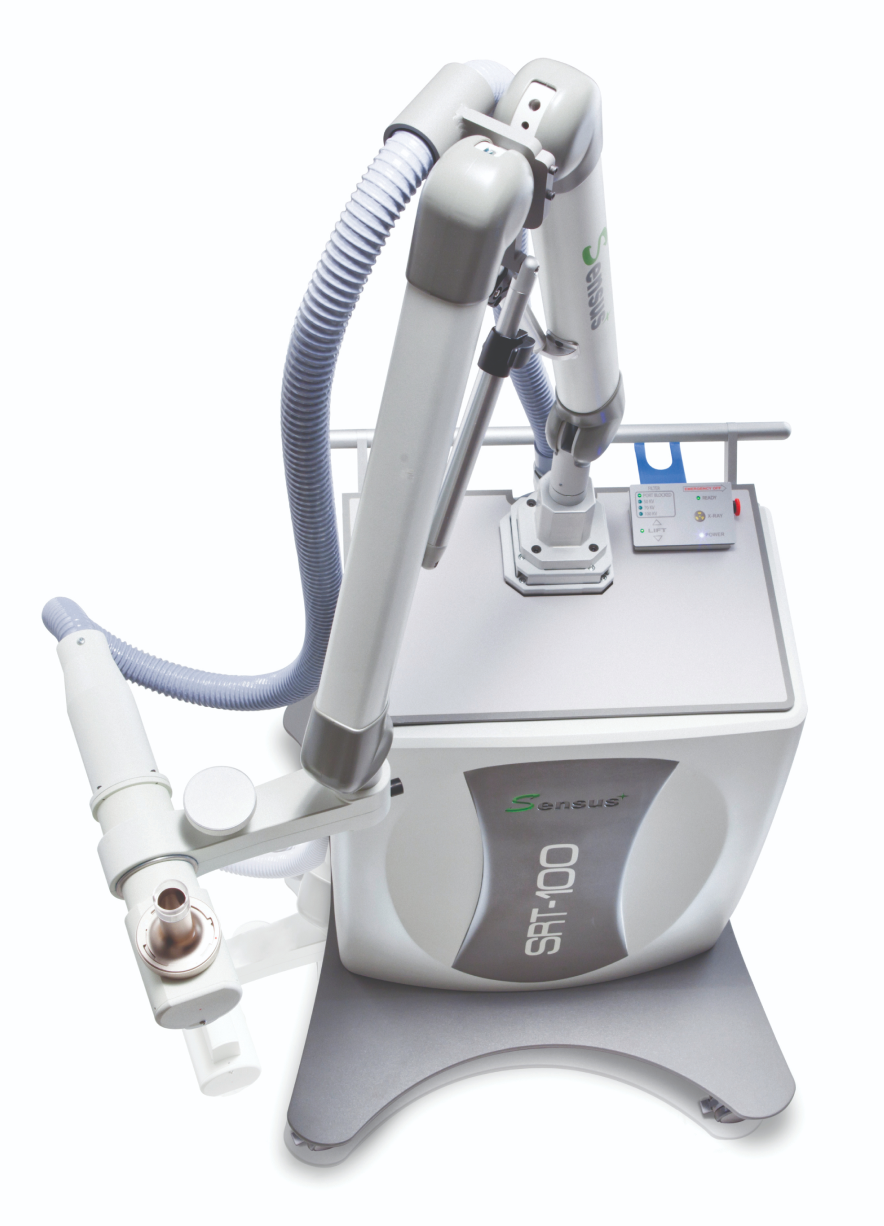
How Radiation For Skin Cancer Works
SRT uses low-energy, targeted radiation — similar in strength to a dental X-ray — to destroy cancer cells at the surface of the skin.
No cutting, bleeding, or stitches are involved.
The treatment is painless and performed entirely in-office.
The radiation is delivered over multiple short sessions (typically 2–3 times a week for 10–15 visits).
Modern ultrasound-guided SRT technology allows your dermatologist to precisely target the cancer cells while preserving the surrounding healthy tissue. This results in excellent cosmetic outcomes and high cure rates, comparable to surgery in select cases.
What to Expect During and After SRT
The treatment area may become slightly red or irritated midway through therapy as the body’s immune response activates.
Mild flaking or crusting is possible but temporary.
No downtime, stitches, or post-surgical wound care are required.
Several weeks after completing therapy, the treated skin usually returns to a smooth, clear appearance.
Dr. Patel explains:
“Patients often appreciate that SRT is entirely non-surgical. It’s especially helpful for those who want to avoid a scar or who aren’t good candidates for surgery due to age, medical conditions, or are on certain blood thinners.”
How Dermatologists Decide: Mohs or SRT?
The process begins with a clinical evaluation and skin biopsy. During your visit, your dermatologist examines the lesion visually and may use a dermatoscope, a handheld magnifying device that reveals surface and pigment details invisible to the naked eye. If the spot looks suspicious for basal cell or squamous cell carcinoma, a biopsy is performed — usually the same day.
Once the biopsy results return from the pathology lab (typically within 7–10 business days), your dermatologist reviews them carefully, looking at:
1. Type and Depth of Skin Cancer
Basal and squamous cell carcinomas may be treated with either Mohs or SRT, depending on depth.
Melanoma and deeper tumors always require surgical removal — SRT is not used for melanoma.
2. Location on the Body
Areas with high cosmetic or functional importance (face, ears, eyelids, lips, nose, hands, genitals) benefit from Mohs surgery for precision and tissue preservation, though some scarring is expected.
On the other hand, for difficult-to-repair areas, like the nose, ears, eyelids, lips or scalp, SRT may be ideal to avoid complex surgical closures and scarring.
3. Age and Overall Health
Older adults or patients with underlying medical conditions may prefer SRT due to its non-invasive nature and lack of anesthesia or sutures.
Younger, healthy patients often choose Mohs for definitive, one-time treatment.
4. Success Rates and Recurrence Prevention
Mohs surgery boasts cure rates up to 99% for primary basal and squamous cell carcinomas.
SRT has cure rates of 90–95%, depending on tumor type and location, with recent studies showing even higher cure rates using Image Guidance. This is the technique performed in our office.
Both offer long-term control when used appropriately and monitored with regular skin exams.
5. Cosmetic Outcome and Personal Preference
Patients who prioritize scar minimization may lean toward SRT for small, superficial cancers. Others prefer Mohs for its immediate confirmation of complete cancer removal in a single visit.

Timeline and Coordination of Care
From start to finish, the decision process usually takes one to two weeks, depending on lab turnaround time. Here’s a typical sequence:
- Initial Evaluation: The dermatologist examines the lesion, performs a biopsy, and photographs the area for records.
- Pathology Results (5–10 days): The dermatopathologist analyzes the tissue and sends a detailed report.
- Treatment Planning Visit: The dermatologist reviews the pathology, discusses available options (Mohs or SRT), and makes a personalized recommendation.
- Scheduling Treatment: Depending on the choice, the procedure or therapy can often begin within days after the plan is finalized.
For more complex or aggressive skin cancers, Dr. Patel may consult with a radiation oncologist (for SRT) or a Mohs surgeon to ensure the best multidisciplinary approach.
This process is deliberately thorough but efficient — designed to balance accuracy with minimal waiting time, so patients can move forward quickly with confidence and peace of mind.
To Summarize: Common Questions About Mohs Surgery and SRT Treatment for Skin Cancer
- How soon will I know which skin cancer treatment I need?
After your skin cancer biopsy, the pathology results usually arrive within 7 to 10 business days. Once your dermatologist reviews the report, you’ll be contacted promptly to discuss next steps. In most cases, the treatment plan — whether Mohs surgery or SRT — is finalized within one to two weeks of your biopsy, allowing you to start treatment quickly.
- Is Mohs surgery or SRT painful?
Both Mohs surgery and SRT treatment for skin cancer are designed to be as comfortable as possible. Mohs surgery is performed under local anesthesia, so you’ll feel only mild pressure but no pain during the procedure. SRT involves no needles, no cutting, and no anesthesia — patients typically describe it as completely painless, similar to a brief X-ray session.
- Will my treatment leave a scar?
Because Mohs surgery involves removing skin tissue, some degree of scarring is expected, though most heal beautifully with proper wound care. The advantage of Mohs is that it removes only the tissue necessary to clear the cancer, minimizing cosmetic impact. SRT, on the other hand, is a non-surgical treatment, so it typically leaves little to no visible scarring once the skin fully heals.
- How effective are Mohs and SRT treatments?
Both options are highly effective when used for the right type of skin cancer. Mohs surgery offers the highest possible cure rate — up to 99% for many basal and squamous cell carcinomas. SRT achieves cure rates between 90–95%, and is especially useful for patients who prefer a non-invasive alternative or have medical conditions that make surgery difficult.
- What happens after my treatment is finished?
After completing your Mohs surgery or SRT treatment, you’ll have regular follow-up visits to monitor healing and check for any signs of recurrence. Most patients heal completely within a few weeks, and long-term outlook is excellent. Dr. Patel encourages annual full-body skin exams to ensure ongoing skin health and early detection of any new or recurring lesions.
The Goal: Confidence Through Clarity
Understanding your dermatologist’s reasoning helps remove the mystery from the treatment process. At Aesthetic Dermatology Associates, we take the time to explain why a particular option is right for you — based on evidence, safety, and your personal goals.
Dr. Patel notes:
“No two skin cancers — or patients — are the same. My recommendation always comes down to one question: which treatment will give this person the best long-term outcome with the least disruption to their life?”
About the Author
Dr. Patel is a board-certified dermatologist specializing in medical, surgical, and cosmetic dermatology. As a Clinical Instructor at the VA Medical Center – University of Pennsylvania in Philadelphia, he mentors future dermatologists and has published research in leading medical journals.
At Aesthetic Dermatology Associates, with offices in Paoli and Media, Pennsylvania, Dr. Patel provides expert care for skin cancer diagnosis and treatment, including Mohs surgery and Superficial Radiation Therapy (SRT). His approach combines medical excellence with compassion and clear communication.
Related links
See Dr. Patel’s personal page on our website
Follow Dr. Patel on LinkedIn professional social network
Review Dr. Patel’s rating on US News Health website
Schedule a Skin Cancer Consultation in Paoli or Media, PA
If you’ve been diagnosed with basal or squamous cell carcinoma and want to explore whether Mohs surgery or SRT treatment is right for you, schedule a consultation with Dr. Patel at Aesthetic Dermatology Associates.
Our team will review your biopsy results, discuss your options in detail, and design a treatment plan that fits your medical needs and lifestyle.
What to Do Right After a Skin Cancer Biopsy: First 48 Hours

Explained By Dr. Patel, Board-Certified Dermatologist, serving Paoli & Media, PA
When patients visit us for a skin cancer screening, it’s common for a dermatologist to notice a suspicious mole, lesion, or spot that needs further evaluation. In these cases, a biopsy for skin cancer is often recommended to confirm whether the area is benign, precancerous, or malignant.
From the patient’s perspective, this can be an anxiety-filled moment. The idea of a biopsy—and the waiting that follows—can cause understandable stress. Knowing what a skin cancer biopsy involves, how to care for the area afterward, and what to expect in the first 48 hours can make the process much less intimidating.
What Is a Skin Cancer Biopsy?
A biopsy is a quick, in-office diagnostic procedure in which a dermatologist removes a small tissue sample from a suspicious mole, spot, or lesion for microscopic evaluation by a dermatopathologist. It is the only definitive method to confirm or rule out skin cancer and plays a crucial role in early detection and treatment.
The entire process is performed under local anesthesia and typically takes less than ten minutes. Most patients experience only minor pressure or a brief stinging sensation from the anesthetic and can return to normal activities immediately afterward.
A biopsy may be recommended if you have:
- A new mole or growth that looks different from your others
- A changing lesion that’s growing, itching, or bleeding
- A non-healing sore that persists for weeks
- A rough, scaly patch or pink bump that bleeds easily
- Any area your dermatologist suspects could represent basal cell carcinoma, squamous cell carcinoma, or melanoma
How a Skin Cancer Biopsy Is Performed
A skin biopsy begins with careful cleaning and sterilization of the area. Next, a small injection of lidocaine is given to numb the skin completely.
Depending on the lesion and its depth, your dermatologist will most likely perform one of two common techniques:
Shave biopsy – removes a thin layer of skin and usually requires no stitches.
Punch biopsy – removes a small, deeper cylinder of skin that may need a suture.
After the sample is taken, a protective dressing is applied, and our medical assistant provides written biopsy wound care instructions. At our Paoli and Media, PA dermatology offices, this entire process usually takes just a few minutes and is well-tolerated by patients of all ages.
However, there are two more types of biopsy applied rarely:
Excisional biopsy – removes the entire lesion along with a small margin of normal skin. Typically performed when melanoma is suspected.
Incisional biopsy – removes a portion of a large lesion when full removal isn’t practical at first. Used for diagnostic sampling.
The First 48 Hours After a Biopsy
During the first two days after your skin cancer biopsy, the goal is to protect the area and allow natural healing to begin. Keep the bandage clean, dry, and undisturbed for at least 48 hours.
Dr. Patel explains:
“We usually advise patients to keep the area dry and avoid removing the dressing too early. A little tenderness or redness is completely normal during the first couple of days.”
Because biopsy sites are small, most patients can continue regular activities, including work and light exercise, unless specifically advised otherwise.
You may experience mild soreness, minimal bleeding, or a small scab formation—these are all part of the normal skin biopsy healing process.
If you exercise regularly, this article explains what to expect when resuming physical activity after a biopsy.
Caring for the Biopsy Site After Two Days
After 48 hours, you can begin daily skin biopsy aftercare:
- Gently remove the old bandage—doing so in the shower often helps loosen it painlessly.
- Cleanse the site with mild soap and water, and pat it dry with a clean towel.
- Apply a thin layer of petroleum jelly to keep the wound moist.
- Cover it with a fresh bandage, repeating this once or twice daily for about one week.
Dr. Patel emphasizes:
“Moist wound care leads to faster healing and less scarring. Dry wounds tend to heal more slowly and may leave a noticeable mark.”
Unless otherwise instructed, there’s no need for antibiotic ointment—plain petroleum jelly works best for most skin biopsy wounds.
Waiting for Biopsy Results
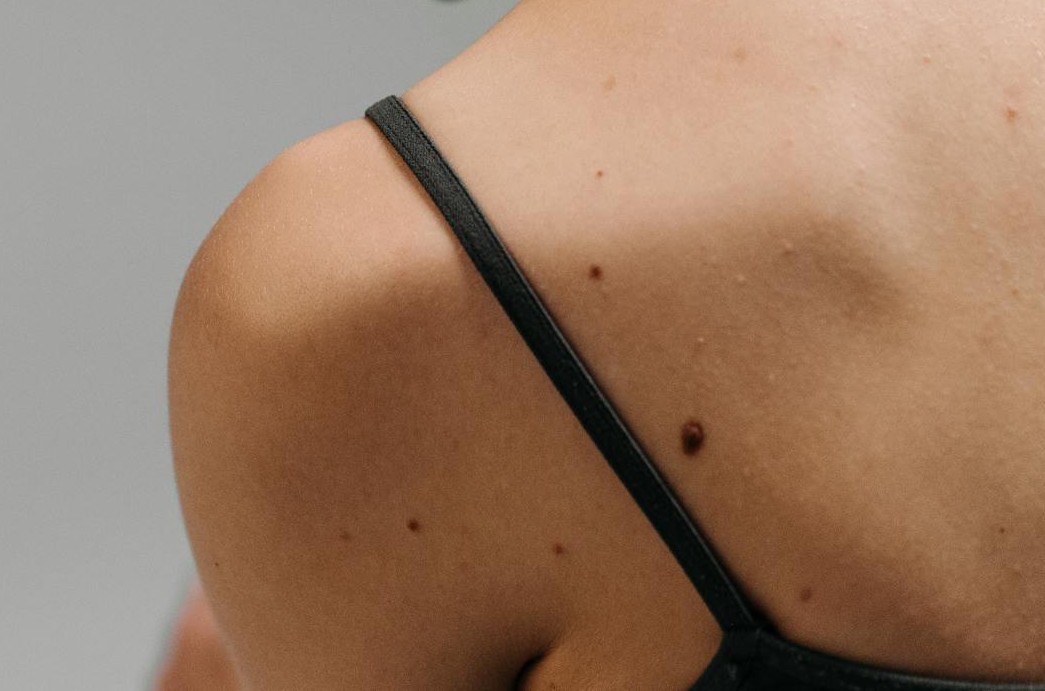
For many patients, the most difficult part of the skin cancer biopsy process isn’t the procedure itself — it’s the waiting. Once your dermatologist sends the tissue sample to the pathology lab, there’s an unavoidable period of anticipation while the cells are examined under a microscope by a board-certified dermatopathologist.
Typically, skin biopsy results are ready within 7 to 10 business days, though the exact timing can vary depending on several factors:
- The laboratory’s workload and processing times
- The type of biopsy performed (shave, punch, or excisional)
- The complexity of the findings — certain cases require deeper staining or secondary review
- Weekends or holidays that may slightly delay turnaround
At Aesthetic Dermatology Associates in Paoli and Media, PA, our team closely monitors every biopsy we submit. We ensure that results are communicated as soon as they’re finalized, following the method you chose during your visit — whether that’s a phone call, secure patient message, or in-person follow-up appointment. If you haven’t received your results after 10 days, you’re always welcome to contact our office. Our staff will immediately check the lab status and provide an update.
What the Biopsy Results Can Tell You
Your biopsy report provides detailed, microscopic information that helps your dermatologist determine the next steps. It typically includes:
- The diagnosis — whether the lesion is benign, precancerous, or malignant
- The type of cells involved (for example, basal cell carcinoma, squamous cell carcinoma, or melanoma)
- The depth and margins of any abnormal cells
- Recommendations for follow-up or treatment
This information guides whether additional treatment is needed, such as complete excision, cryotherapy, topical medication, or Mohs micrographic surgery.
Coping with Anxiety While Waiting
It’s completely normal to feel anxious during the waiting period. Many patients describe checking their phone or email multiple times a day, worried about what the results might say. Dr. Patel encourages patients to remember the following:
Most skin cancer biopsies come back benign. A large percentage of biopsied spots turn out to be harmless moles, keratoses, or other noncancerous growths.
Early detection saves lives. Even if the biopsy confirms skin cancer, it usually means it was found early — when treatment success rates are highest.
You are not alone. Our team is available to answer questions or provide reassurance while you wait. Sometimes, a quick conversation can relieve much of the uncertainty.
Avoid searching for symptoms online. Each biopsy is unique; general internet results can increase worry rather than offer clarity.
When to Contact Your Dermatologist
Complications after a skin biopsy are uncommon, but it’s important to call your dermatologist if you experience:
- Persistent bleeding that doesn’t stop with firm pressure
- Increasing redness, swelling, or pain
- Pus or drainage from the wound
- Fever or expanding redness
Dr. Patel notes:
“If something doesn’t seem right, don’t hesitate to call our office in Paoli or Media. Most post-biopsy concerns are minor and easy to treat, but it’s always better to check in early.”
The Skin Cancer Biopsy Healing Timeline
Healing from a biopsy generally takes one to two weeks. Shave biopsies heal faster, while punch biopsies may require slightly more time. During the healing process, the site may appear pink or red before gradually fading to your natural skin tone.
To promote smoother healing:
- Avoid picking or scratching the area.
- Protect the biopsy site from direct sunlight.
- Once healed, apply broad-spectrum sunscreen daily to help minimize scarring.
- If a small scar remains, cosmetic treatments such as laser resurfacing or microneedling can improve its appearance later on.

To Summarize: Common Questions After a Biopsy for Skin Cancer
- How long does it take for a skin cancer biopsy to heal?
Most skin biopsy sites heal within 7–14 days. Shave biopsies may close quickly, while punch biopsies with stitches may take slightly longer. Proper wound care and sun protection help minimize scarring.
- Can I shower after a skin biopsy?
You can shower gently after 48 hours once your dermatologist instructs you to remove the dressing. Use mild soap, avoid scrubbing, and reapply petroleum jelly with a new bandage afterward.
- What should I do if my biopsy site bleeds?
Apply firm pressure with a clean tissue or gauze for 10–15 minutes. If bleeding doesn’t stop or soaks through the bandage, call your dermatologist right away.
- When will I get my biopsy results?
Pathology results are usually ready within 7–10 business days. Aesthetic Dermatology Associates contacts you promptly according to your chosen communication method.
- Is it normal to feel anxious after a biopsy for skin cancer?
Yes—many patients feel nervous while waiting for results. Remember, most biopsies reveal non-cancerous findings, and early detection leads to excellent outcomes if treatment is needed.
Final Thoughts from Dr. Patel
“A biopsy for skin cancer is one of the most important tools we have to protect your health. It’s quick, safe, and gives us the answers we need to create an effective treatment plan. With proper care and a little patience, the biopsy site will heal, and you can move forward with confidence.”
Schedule a Follow-Up or Skin Cancer Screening in Paoli or Media, PA
If you’ve recently had a biopsy or noticed a new or changing mole, schedule a follow-up with Dr. Patel at Aesthetic Dermatology Associates. Our dermatology clinics in Paoli and Media, Pennsylvania provide expert diagnosis, personalized treatment, and compassionate follow-up care.
About the Author

Dr. Patel is a board-certified dermatologist with advanced training in medical, surgical, and cosmetic dermatology. An Adjunct Associate Professor at the University of Pennsylvania Perelman School of Medicine in Philadelphia, he has authored peer-reviewed research and mentored future dermatologists.
At Aesthetic Dermatology Associates, Dr. Patel specializes in skin cancer diagnosis and treatment, medical dermatology, and patient education. He proudly serves the communities of Paoli, Media, and the greater Philadelphia Main Line area, providing compassionate, evidence-based dermatologic care.
Related links
See Dr. Patel’s personal page on our website
Follow Dr. Patel on LinkedIn professional social network
Review Dr. Patel’s rating on US News Health website
Visit Our Locations
Media, PA
| Mon: | 7:30 am - 5:30 pm |
| Tue: | 8:00 am - 4:00 pm |
| Wed: | 7:30 am - 4:00 pm |
| Thu: | 7:30 am - 4:00 pm |
| Fri: | 7:30 am - 1:00 pm |
Paoli, PA
| Mon: | 8:00 AM - 4:30 PM |
| Tue: | 8:00 AM - 4:00 PM |
| Wed: | 8:00 AM - 5:30 PM |
| Thu: | 8:00 AM - 4:30 PM |
| Fri: | 8:00 AM - 5:00 PM |
Stay Informed with our Newsletter

Book Your Appointment Today!
Choose the option that works best for you:
Prefer to speak with someone? Call or text us:

Media, PA Office - Call or Text (610) 566-7300

Paoli, PA Office - Call or Text (610) 647-4161
Want to book online now? Select a provider below:
Note: Self-scheduling is currently available for Dr. Ko & Bridget Lolli. For all other providers, please call or text the office.